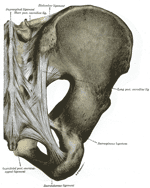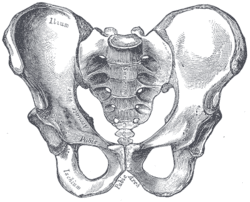
So treatment almost sometimes became taking a shot in the dark as I never truely felt confident in my exam findings. This led me to perform treatments and progressions of patients based on trial and error rather than because of exam findings. (Photo from Wikipedia)
Assessing the Sacroiliac Joint
Treating this way, to me, is a huge pet peeve, so I started to research the area to gain more comfort in my SI joint examination. I found some interesting research regarding palpation, SI joint motion, and provocative testing. Here are some of the things that I found along that way that really helped me get better at diagnosing SI joint pain, hope it helps you too.
Palpating the SI Joint
One of the simplest methods of assess the SI joint is palpation. However, the reliability and validity of palpating the SI joint has come into question in recent years. Several studies have been published showing poor inter-tester reliability for static SI joint palpation, including a nice study from Holgren and Waling.
McGrath has published an interesting article, entitled “Palpation of the sacroiliac joint: an anatomical and sensory challenge” in which the concept of SI joint palpation is scrutinized. It is an interesting paper, that certainly makes you think. In the paper, the author describes the several layers of tissue that sit between the skin and the posterior SI joint, which is 5-7cm deep to the skin, and the inherent challenge of both reliability and validity of palpating something so deep.
Assessing SI Joint Motion and Symmetry
Assessing the amount of SI joint motion and the symmetry of the SI joint itself is a very commonly performed technique during SI joint examination. This method of examining the SI joint is popular and accepted, despite the lack of research supporting the technique.
Based on the above information regarding palpating the SI joint, one would question the ability to palpate AND now accurately assess motion in addition. If palpation has poor reliability, this automatically makes assessing motion difficult.
Freburger and Riddle performed a literature review looking at our ability to perform SI joint motion testing. They found poor inter-tester reliability, low sensitivity, and low specificity in several commonly performed tests. This is a particularly interesting article to read if you have interest in this area.
Another study from Robinson et al had similar conclusions, stating that SI joint motion palpation tests have poor inter-tester reliability.
Riddle and Freburger in another study noted that the ability to detect positional faults of the SI joint also has poor reliability.
Thus it appears that the reliability and validity of assessing SI joint symmetry and motion may be too poor to be used clinically. The amount of motion of the SI joint motion is extremely small, perhaps less than 2mm and 2 degrees of translation and rotation. This makes detecting patholgoical movement extremely challenging.
However, I still think symmetry and motion assessment may be a valuable component of the SI joint examination in the case of significant malalignment and pathology, and still should be assessed. Just realize that you are looking to “rule in” more significant pathology. I would not “rule out” SI joint dysfunction based solely on symmetry and motion assessment.
Location of SI Joint Symptoms
Van der Wurf et al (2006) published an interesting study looking at the location of symptoms reported in patients with SI joint pain and dysfunction. In the study, the authors performed local SI joint injections to block the patients’ pain. The authors found that:
- All subjects that responded to the SI joint block had symptoms located at the Fortin area (3cm horizontally by 10 cm vertically inferior to the PSIS)
- All subjects that did NOT respond to the SI joint block had symptoms at the Tuber area (just inferolateral to the ischial tuberosity)
Again, I wouldn’t rule in or rule out SI joint dysfunction based on this alone, but it appears that if you DO have pain at the Fortin area AND do NOT have pain at the Tuber Area, you may be experiencing SI joint pain.
SI Joint Provocative Tests
Two recent studies by Laslett et al and Van der Wurff et al have demonstrated that there probably isn’t one perfect SI joint provocative test that we can perform to definitively diagnose SI joint pain or dysfunction. Basically, there is no “gold standard” such as using the Lachman test for ACL tears in the knee.
However, by performing several tests together, you can increase your sensitivity and specificity of detecting SI joint dysfunction.
Combining the two studies, there are 5 provocative tests to perform when attempting to diagnose SI joint pain:
- Gaenslen
- FABER / Patrick’s test
- Thigh thrust / femoral shear test
- ASIS distraction (supine)
- Sacral compression (sidelying)
Laslett et al report that the accuracy of detecting SI joint dysfunction is increased with at least 3 of the 5 tests are positive. Furthermore, if all 5 tests are negative, you can likely look at structures other that the SI joint. Van der Wurff et al report that if at least 3/5 of these tests were positive, there was 85% sensitivity and 79% specificity for detecting the SI joint as the source of pain. Interestingly, another study by Kokmeyer et al agreed with the previous findings, but also noted that the thigh trust test alone was almost as good at detecting SI joint dysfunction as the entire serious performed together.
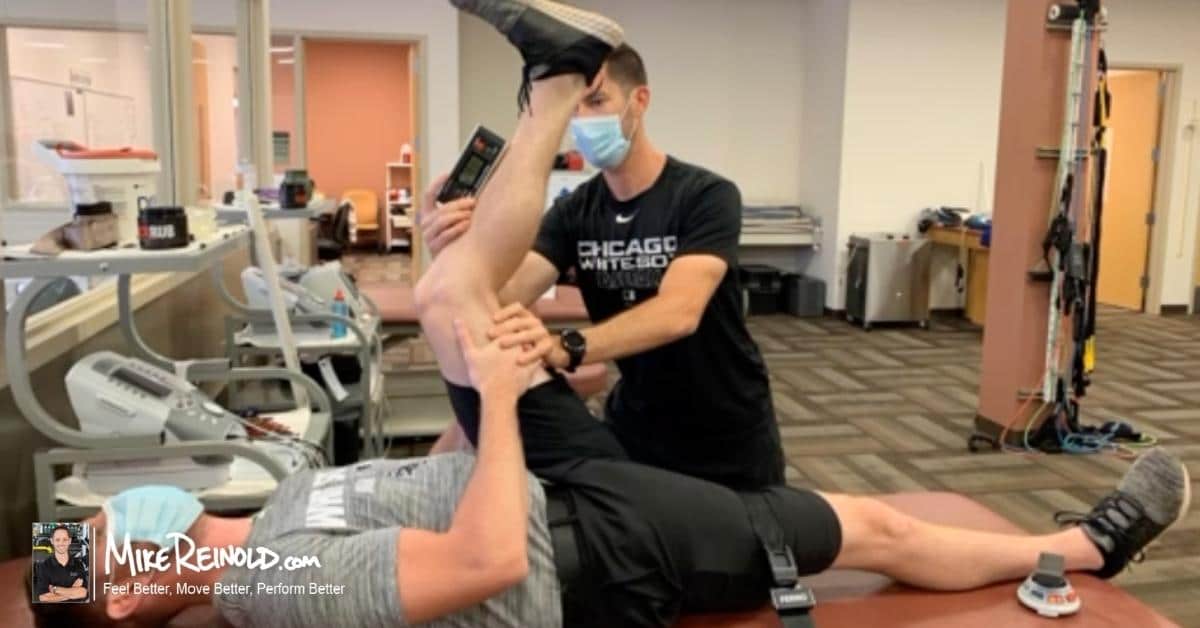
It seems like performing a series of provactive SI joint tests is better than one true test in isolation, though I would specifically emphasize the thigh thrust test. In my experience, you have to use a decent amount of force during the thigh thrust technique to avoid missing a positive provactive sign.
In an attempt to find good demonstration videos on youtube of these techniques, I came across Harrison Vaughn’s excellent videos (I mentioned Harrison in the past and recommend you also check out his website). Great job and thanks for sharing Harrison! These are the tests recommended by the above authors to use together:
Gaenslen Test
FABER / Patrick Test
Thigh Thrust / Femoral Shear Test
ASIS Distraction
Sacral Compression
The Best Tests for SI Joint Pain
I will admit that I am not a SI joint expert, so I am interested in hearing the opinion of my readers that deal with a lot of SI joint dysfunction. It appears that palpation, symmetry, and motion testing of the SI joint may have concerns in regard to reliability and validity.
Some things to keep in mind when assess the sacroiliac joint:
- It is difficult to palpate the deep SI joint, making reliability and validity challenging
- The reliability of assessing symmetry, SI joint motion, and SI joint position also has poor reliability
- Pain along the Fortin Area without pain in the Tuber Area may indicate SI joint pain
- A series of provocative SI joint tests yields better results that performing tests in isolation, with at least 3/5 positive tests demonstrating the highest accuracy of detecting SI joint dysfunction
Based on some of the research above, we should all consider the location of symptoms and a series of provocative testing when attempting assessing the sacroilliac joint and diagnosis SI joint pain and dysfunction.