Today’s post is part 2 of a series by Shaun Logan, DPT, on concussions in sports and the role of rehabilitation. Please be sure to read part 1 of the series on concussions in sports regarding the risks and recovery process following a concussion.
The Role of Rehabilitation in Concussion Management
It may be thought that the athlete with a concussion should not start any treatment until completely asymptomatic at rest, however this does not necessarily have to be the case. The athlete should not show any worsening of symptoms at rest. [5] We require that their physician refer the athlete before starting physical therapy. It is necessary for a concussion to be managed with a team approach of the physician, physical therapist, athletic trainer, parent (when applicable), and the patient to best manage the recovery of the athlete.
A rehabilitation specialist is able to evaluate and treat many of the symptoms and problems related to concussions. No two concussions or athletes’ symptoms are the same, so a thorough evaluation is performed and a personalized treatment plan is then designed for the athlete. After the athlete is asymptomatic at rest, or is with extended symptoms, they need to be assessed while performing symptom provoking movements and activities to ensure they have fully recovered, or assess their status in recovery.
Concussions and the Vestibular System
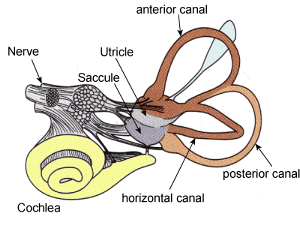
The vestibular system, which includes the inner ear and its connections with the brain, is responsible for sensing head movement, keeping your eyes focused when you move your head, and helping you keep your balance.[6] This is integral in recovery from a concussion, as these movements are very common in reproducing and worsening of symptoms. It is common for an athlete’s symptoms to be reproduced with simple activities such as reading or taking notes in class. They must be progressed and monitored appropriately by a health care professional, which in turn can decrease their length of symptoms. [6]
The vestibular aspect appears to mostly involve vestibulo-ocular reflex, smooth pursuit, saccades, tracking, and convergence/divergence mostly. Just as with any sports injury and dealing with an athlete, they need to be pushed harder and progressed in different ways that a lot of general outpatient patients do not require. Continue to challenge the athlete.
As rehabilitation specialists, we can also address neck problems, including tightness, soreness, and pain following a concussion. Addressing these issues will assist in reducing headache symptoms. At physical therapy we will also address any other possible injuries or limitations the athlete may have sustained. This can be initiated while the athlete is still symptomatic at rest. Though, these are not highly statistically reported symptoms, they will occur in some athletes.
Rehabilitation Specialists will focus on the symptoms and limitations observed during the evaluation and continually as the athlete is being treated.
Treatment sessions will focus on, but are not limited to:
- vestibular rehab for reducing dizziness
- ocular reflexes and tracking
- balance/proprioception
- cranial nerve assessment
- change of position
- hand-eye coordination
- body mechanics and posture
- neck stabilization
- incremental progression of exertion with heart rate monitoring
- sport specific training
Return to Play Following a Concussion
The majority of athletes with concussive symptoms will completely recover within 7-10 days. However, they still need to be tested for any concussion symptoms with balance, vestibular activities, and through a progression of exertional activities to assess for symptoms. Simply because the athlete may not have symptoms at rest, does not automatically mean they can return to sport without experiencing symptoms, such as dizziness, headaches, vomiting, etc. This is why the athlete must be gradually progressed through stages of exercise and exertion to assess for PCS.
The more involved rehabilitation will occur for individuals who have continued symptoms for longer periods of time.
As the athletes’ symptoms improve, which will be closely monitored by the rehabilitation specialist, they will be gradually and properly progressed through physical activity towards return to sport, or normal level of activity, using a graded exercise approach for return to play. (*See below for two examples of 5 step graduated return-to-play protocols.)
The timing of the progression through the stages depends on how long the athlete had symptoms at rest. The longer the symptoms at rest, the slower the progression through the stages. This will be determined by the physical therapist in conjunction with the physician, athletic training, and feedback from the patient. Typically, the athlete should be asymptomatic for approximately 24 hours between stages prior to progressing.
A lot of focus of the treatment will be the athletes’ ability to respond to multiple stimuli simultaneously. An example of a high level task would be having the athlete balance on an unstable object while catching and throwing balls to different specified targets. This exercise incorporates several systems including somatosensory/proprioception, neuromuscular, musculoskeletal, vestibular, ocular motor, and cognition.
Ultimately, the overall goal is to properly manage and progress the athlete towards return to his/her sport as safely as possible to reduce risks of further and worse consequences. It is important to remember that each athlete is different, as is each concussion. Treat the symptoms with which the athlete presents, tailor the plan of care to their needs whether it be reading or sport specific movements. Athletes need to be challenged in ways the average person does not, so do not be afraid to push them (while in a more controlled environment) when appropriate to challenge the athlete and try to provoke symptoms. But at this point…err on the side of caution.
Return to Sport Progressions Following a Concussion
Below are two example progressions to return to sport activity following a concussion.
Resumption of Physical Activity progression from Concussion Health [6]:
- Light aerobic exercise (e.g., walking or stationary cycling) at 30-50% heart rate for 15-25 min; Vestibular/visual/balance exercises as needed.
- Sport specific training (e.g., running drills, agility skills) at 50-70% heart rate for 25-40 min; advanced vestibular/visual/balance exercises as needed.
- Non-contact training drills at 70-90% heart rate for >45 min
- Full contact drills
- Game play
*5 Step Graduated Return-To-Play: [4]
- 20 minute stationary bike ride (1-14 mph)
- Interval bike ride: 30 sec sprint (18-20 mph/10-14 mph)/ 30 second recovery x10; and BW circuit: Squats/push ups/sit-ups x20 sec – x3
- 60 yard shuttle run x 10 (40 sec rest); plyometric workout: 10 yd bounding/10 medicine ball throws/10 vertical jumps x 3; and non-contact, sport specific drills for approximately 15 minutes
- Limited, controlled return to full-contact practice
- Full sport participation in a practice
As you can see, there is more than one way to skin a cat and both progressions look appropriate. The take away message is to assure you are gradually progressing the patient while monitoring symptoms at each level. Then, be sure to customize the progression for the specific goals and activities of each patient.
References
- University of Pittsburg Medical Center. (2011)
- University of Pittsburg Medical Center. (2011)
- McCory P, Meeuwisse W, Johnston K, et al. (2009) Consensus Statement on Concussion in Sport: the 3rd International Conference on Concusion in Sport held in Zurich, November 2008. Br J Sports Med; 43: i76-i84
- Guskiewicz, K. Concussion and Postconcussive Syndrome: When to Rest, Exercise, or Return to Sport. 2010. APTA Annual Meeting, Boston, MA
- Wallace, B. (2011) Concussion Health: Program
- Mucha, A. Physical Therapist’s Guide to Concussion. American Physical Therapy Association. 3/24/2011
- Wallace, B. Concussion Management Guidelines: Balance 360. By Concussion Health. (2011)
About the Author





