The core stabilization concept keeps being a hot topic for discussions. After more than a decade of core-training frenzy there is still very little evidence that core-training actually produces any positive effects. There is no universally accepted definition of what the make-up and function of the core is.
It all started with the Transversus Abdominis and the abdominal hollowing theory, where people were instructed to pull the belly-button in towards the spine when exercising. It has since been shown that abdominal bracing (tensing the abdominal wall as if preparing for being punched in the stomach) is superior to abdominal hollowing in regards to providing stability for the lumbar spine. Abdominal bracing is good, but it is still approaching the core from the outside in. The abdominal wall is the focus of the training. Real core activation has to come from the inside out.
Definition of Core
When looking up “core” in a dictionary we get descriptions like: centre, nucleus, middle, heart and interior.
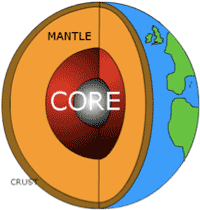
If someone refers to the core of our planet they mean the absolute centre. When people train their core they concentrate on the outer layers of the wall equal to the crust and the mantle.
People have to stop treating the core as a hollow tube and learn how to pressurize the “centre” of the tube instead of just tensing the walls.
How do we pressurize the “centre”?
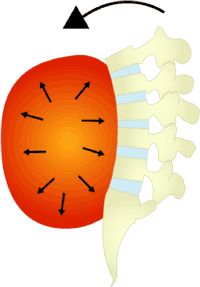
Diaphragm
The diaphragm is the key component to core stability. The diaphragm has to contract first and then the abdominal wall and not the other way around. A too early or too strong contraction of the abdominal wall prevents the diaphragm from descending properly and is therefore counterproductive in stabilizing the spine.
At this point I would like to present the results of two interesting MRI studies of the diaphragm by Professor Kolar and colleagues that demonstrated that the diaphragm has dual functions of respiration and stabilization.
The first study (1) demonstrated that the diaphragm has a postural function that can be voluntarily controlled and is independent upon breathing.
The second study (2) showed that the diaphragm can performed its dual functions of stabilization and respiration simultaneously. The diaphragm can perform the breathing task at a lowered position ensuring that the stabilizing pressure is maintained throughout the breathing cycles. There is a close relationship between the diaphragm and Transversus Abdominis which contributes to the respiratory and postural control.
These two studies pointed out that the activity of the diaphragm during stabilization varies greatly amongst individuals, which supports Kolar’s clinical evidence that individuals with limited capability to contract the diaphragm for stabilization have a higher risk of developing back-pain. The simultaneous activation of the diaphragm’s dual functions is the key to proper core stabilization
It is interesting to note that in the study by Hodges and colleagues which started the core craze, it showed that not only the transversus abdominis but also the diaphragm was activated to stabilize the trunk prior to any limb movement. The transversus got all the attention and turned into the core super-star while the diaphragm got ignored.
Respiratory function of the diaphragm
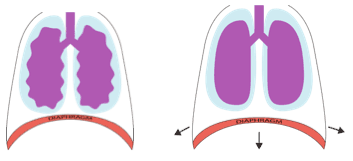
During inspiration the diaphragm contracts and pushes down into the abdominal cavity which decreases the pressure in the thoracic cavity and the lungs fill up with air.
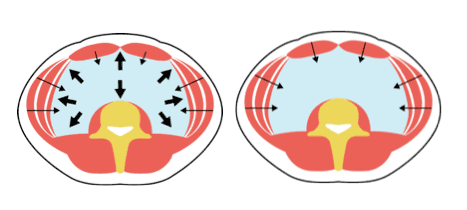
The diaphragm participates in all breathing patterns whether they are ideal or dysfunctional. You cannot avoid using the diaphragm when breathing even if you try, unless there is a medical condition preventing the diaphragm from contracting. The commonly used instruction “breathe with the diaphragm“, has no value. Chest breathing and straight belly-breathing, where only the posterior part of the diaphragm pushes downwards, are two commonly observed dysfunctional breathing patterns, which reduce both the respiratory capacity and core stabilization. In ideal diaphragm contraction the entire diaphragm pushes down into the abdominal cavity and can be observed by an expansion of the lower ribcage and the abdominal wall in all directions.
Assessing diaphragm function
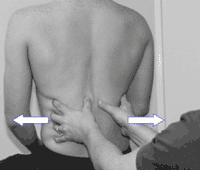
Next, the subject’s ability to pressurize all the way down to the lower part of the abdominal cavity when breathing is assessed, both in laying and sitting (holding the ribcage down assists the activation) .
After that, the postural function of the diaphragm is assessed. Instruct the individual to pressurize all the way down to the bottom of the abdomen while holding their breath. The instructor should be able to feel the pressure against a hand placed at the lower abdomen.
And finally, get the person to breathe all the way down to the lower abdomen and then maintain that pressure while going through normal breathing cycles. The diaphragm is now performing its breathing function at a lower position. This is real core stabilization.
Each of these steps should be properly activated and the testing positions are excellent to use as entry-level exercises. A resistance band can be strapped around the ribcage or the lower abdomen to pressurize against. It is worth spending a fair amount of time ensuring proper activation of the core before progressing to other exercises.
Here is a video, explaining core activation from the inside out:
Once proper activation of the core is achieved, only the individual’s imagination limits the exercise progression. Planks, bird-dogs, dead-bugs would be reasonable next steps. Uni-lateral work is an inventive way of keep challenging the core.
Frequently we see discussions regarding whether to perform core-exercises before or after other exercises. After reading this I hope everybody can see that once the diaphragm is properly activated the core will be trained in all exercises and activities. Proper core-activation is fundamental and should be part of everything we do.
The ability of the core to stabilize the spine and torso is the limiting factor in all exercises. Pay close attention to the signs of proper core activation.
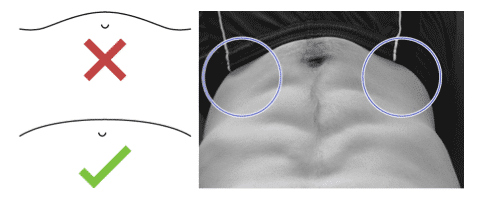
My favourite method of determining if the core is activated is to observe the lower lateral abdominal wall. If there are concavities the core is not properly activated. Concavities indicate a Rectus Abdominis dominant pattern.
The contour of the abdominal wall should take on a balanced, slightly rounded appearance which should be maintained throughout performing the exercise with normal respiration.
Some individuals cannot activate the diaphragm properly by themselves and I would recommend they seek assistance from a DNS or Postural Restoration Institute trained Practitioner. Practicing with faulty patterns will only reinforce the dysfunction.
Core-stabilization has to come from the inside out and is controlled via the diaphragm. I recommend anyone who is interested in improving their performance and preventing low back pain to spend the required time to properly activate the core. It is really worth it. I have had experienced Strength athletes achieve new PB’s straight after we have activated their core.
References:
1- Kolar P, Neuwirth J, Sanda J, Suchanek V, Svata Z, Pivec M. Analysis of diaphragm movement during tidal breathing and during its activation while breath holding using MRI synchronized with spirometry. Physiol Res 58:383-392, 2009
2- Kolar P, Sulc J, Kyncl M, Sanda J, Neuwirth J, Bokarius AV, Kriz J, Kobesova A. Stabilizing function of the diaphragm: dynamic MRI and synchronized spirometric assessment. J Applied Physiol Aug 2010
About the author: