As a general rule of thumb, we should probably consider that many of our traditional “injuries” that seem to be relentless and not responsive to treatments may actually be coming from elsewhere in the body. Think back to how patellofemoral pain has been referred to as “the black hole” of orthopedics and how surgery and rehabilitation to correct patella alignment is often unsuccessful. Perhaps patellofemoral pain is actually just a symptom and not the source of dysfunction.
Below are what I have found to be 3 common “injuries” that may actually just be symptoms from dysfunction somewhere else within the kinetic chain. There are many more than 3, but these are likely to be some of the most common that you may encounter. Feel free to leave a comment of more examples that you have encountered. Furthermore, all three fit into the kinetic chain ripple effect theory as the source of dysfunction is pretty close to the location of symptoms
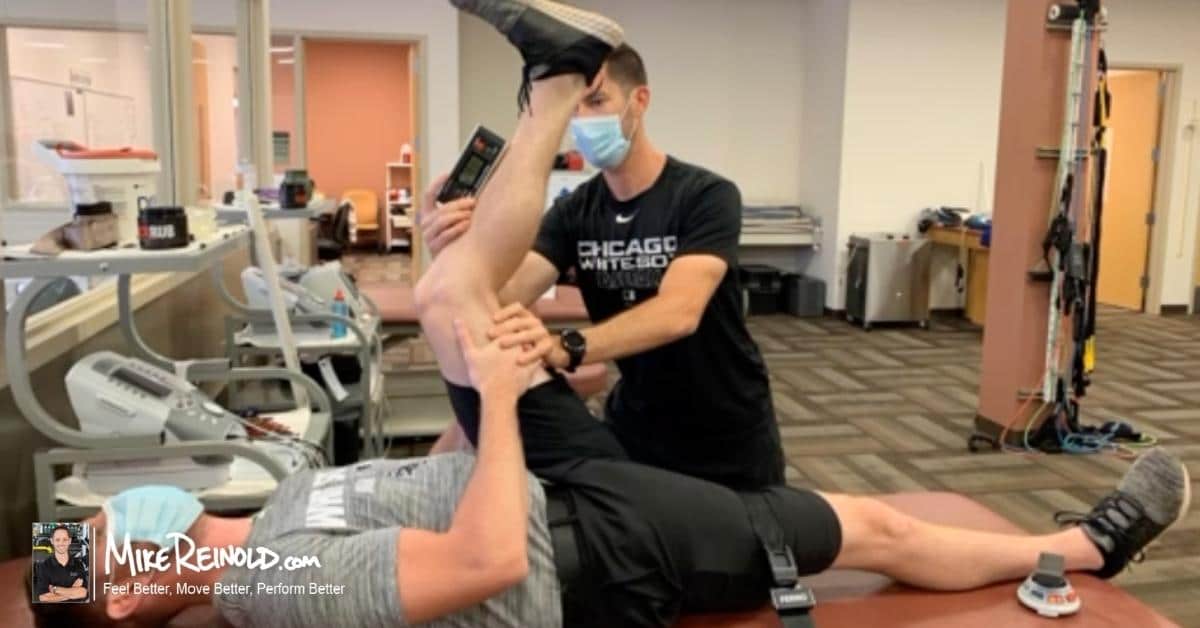
Groin Pain – Source: Hip Joint
I have to admit that in my career I have been stumped by groin strains that seem to be difficult to treat or frequently reinjured. I am sure we have all seen this in our practices, groin pain that doesn’t really look like a groin strain, but what is it? As our understanding of the hip has improved, we find that many people with intra-articular hip joint pathology present with groin pain, which is a common pain referral pattern from the hip joint.
Next time you have a patient with groin pain, clear the hip, you’ll be surprised how many times we find that the symptoms are coming from the hip and that will drastically change our treatment program.
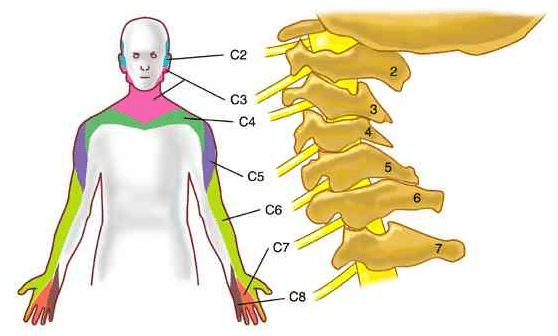
Lateral Epicondylitis – Source: Cervical Spine
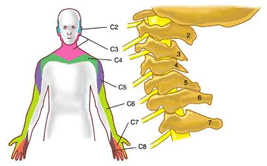
Patellofemoral Pain – Source: The Hip
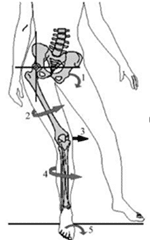
Take Home Message
I’m sure that many of my readers have observed all of the above findings. Please do comment and add more examples. So what is the take home message? For the younger clinicians in the audience, I guess it would have to be that we should probably take a step back a rethink all of the injuries that we see that we consider “difficult to treat” or “unrelenting” such as lateral epicondylitis and patellofemoral pain. Maybe we need to think of the bigger kinetic chain principle. Perhaps we are only treating the symptoms and not the true source of the dysfunction. So next time you seem to have a patient that is not responding to your treatments, take a step back, re-evaluate and assess elsewhere in the kinetic chain and make sure that you haven’t missed the true source of the person’s symptoms.