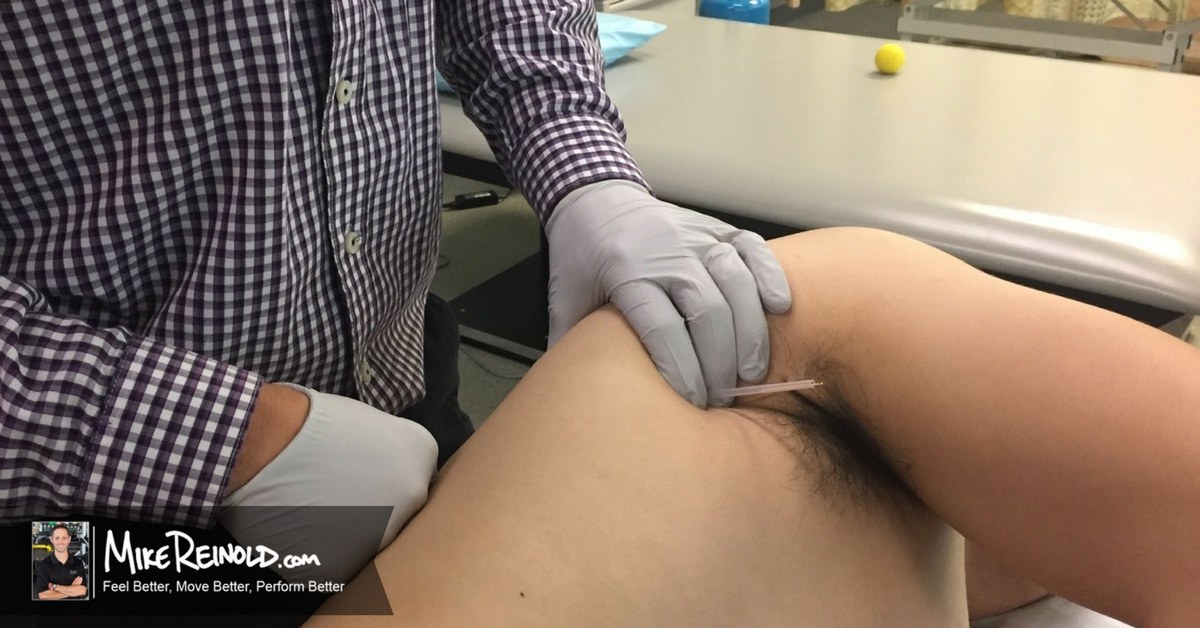
This week’s article is a guest post from Michael Infantino. Michael reached out to me on Facebook and sent me the below videos of a patient’s improvement in scapular winging after dry needling the serratus anterior.
I wanted to share the below article that Michael wrote showing the videos, but also talk about how trigger points may be involved.
I’m not sure what to make of these videos, if trigger points are involved, or exactly how dry needling the serratus anterior helped this patient’s winging. But I am sure that I was impressed with the results. I wish we knew more about the reasoning and mechanism, but in the meantime I’m happy we can help people feel and move better.
Dry Needling for Scapular Winging
Can we correct scapular winging in a matter of minutes? This obviously depends on the cause of the scapular winging.
It is well documented that injury to the long thoracic nerve or cervical spine may lead to medial border scapular winging or dyskinesia of the scapula (Meininger, 2011). These are always challenging. Ruling out neuromuscular cause can be done with a nerve conduction velocity test or EMG.
But a recent patient of mine, made me think…
Research has continually shown that muscles with trigger points demonstrate the following:
- Altered muscle activation patterns on EMG (Lucas, 2010; Wadsworth, 1997)
- Reduced muscle strength (Celik, 2011)
- Accelerated muscle fatigue (Ge, 2012)
- Reduced antagonist muscle inhibition (Ibarra, 2011)
- Increased number of trigger points on the painful side (Alburquerque-Sendin, 2013; Bron, 2011; Fernandez-de-las-Penas, 2012; Ge, 2006; Ge, 2008)
Appreciating these findings would lead most to conclude that treatment of trigger points could improve scapular mobility and timing. This was my immediate thought when I noticed a significant medial border scapular winging while watching my patient raise and lower his arm.
It wasn’t until I read this research that I began using dry needling to do more than just manage pain. The results seen following dry needling to the serratus anterior were remarkable.
After seeing this amount of scapular winging, I dry needled his serratus anterior muscle. Note the remarkable improvement:
How Trigger Point Dry Needling May Impact Scapular Winging
It is well documented that appropriate muscle activation patterns (MAP) surrounding the shoulder is necessary for efficient and pain free mobility (Lucas, 2003). Lucas and group actually gauged the effect of trigger point dry needling on MAP in subjects with latent trigger points (LTrP).
“Latent myofascial trigger points (LTrPs) are pain free neuromuscular lesions that are associated with muscle overload and decreased contractile efficiency” (Simons et al., 1999, p. 12). MAP’s of the upper trapezius, serratus anterior, lower trapezius, infraspinatous and middle deltoid were compared in a group with LTrP’s and one without. Following surface EMG, the LTrP’s were treated with trigger point dry needling. Surface EMG was performed after treatment as well.
Findings from this study were as follows:
- Muscle activation of the upper trapezius in the LTrP group pre-treatment.
- Early activation of the infraspinatous in the LTrP group pre-treatment.
- Increased variability of muscle activation in all muscles assessed in the LTrP group pre-treatment compared to the control group.
- Altered MAP of distal musculature (infraspinatous and middle deltoid) were consistent with co-contraction, a finding that has been attributed to increased muscle fatigability (Chabran et al., 2002).
- Improved muscle activation times in the LTrP group following dry needling.
- Significant decrease in the variability of muscle activation in the LTrP group following dry needling, except for the serratus anterior.
- The serratus anterior and lower trapezius showed increased variability in both the control and LTrP group, which may be why the results did not reach significance. This is also consistent with the latest research in JOSPT that found dyskinesia to be normal in asymptomatic populations. (Plummer, 2017).
Based on the both my clinical experiences and the research presented in this paper, it would seem highly valuable to focus on the treatment of trigger points to restore muscle activation patterns surrounding the shoulder complex.
Being able to press the “reset button” on a muscle is important for re-establishing normal muscle activation patterns prior to exercise. Inclusion of other manual therapy and exercise techniques is important for optimizing function of the local musculature (range of motion, hypertrophy, strength and endurance).
No research that I am familiar with has compared dry needling to other manual therapy techniques for restoring MAP in muscles adjacent to the shoulder. Future research that compares various trigger point treatments for restoration of normal MAP would be beneficial.
About the Author
Dr. Michael Infantino, DPT, is a physical therapist who works with active military members in the DMV region. You can find more articles by Michael at RehabRenegade.com.
References
- Alburquerque-Sendin, F., Camargo, P.R., Vieira, A., Salvini, T.F., 2013. Bilateral myofascial trigger points and pressure pain thresholds in the shoulder muscles in patients with unilateral shoulder impingement syndrome: a blinded, controlled study. Clin. J. Pain 29 (6), 478e486.
- Bron, C., de Gast, A., Dommerholt, J., Stegenga, B., Wensing, M., Oostendorp, R.A., 2011a. Treatment of myofascial trigger points in patients with chronic shoulder pain: a randomized, controlled trial. BMC Med. 9, 8.
- Chabran, E., Maton, B., Fourment, A., 2002. Effects of postural muscle fatigue on the relation between segmental posture and movement. Journal of Electromyography and Kinesiology 12, 67–79.
- Celik, D., Yeldan, I., 2011. The relationship between latent trigger point and muscle strength in healthy subjects: a double-blind study. J. Back Musculoskelet. Rehabil. 24 (4), 251e256.
- Cummings, T.M., White, A.R., 2001. Needling therapies in the management if myofascial trigger point pain: a systematic review. Archives of Physical and Medicine and Rehabilitation 82, 986–992.
- Ge, H.Y., Arendt-Nielsen, L., Madeleine, P., 2012. Accelerated muscle fatigability of latent myofascial trigger points in humans. Pain Med. 13 (7), 957e964.
- Ge, H.Y., Fernandez-de-las-Penas, C., Arendt-Nielsen, L., 2006. Sympathetic facilitation of hyperalgesia evoked from myofas- cial tender and trigger points in patients with unilateral shoul- der pain. Clin. Neurophysiol. 117 (7), 1545e1550.
- Ge, H.Y., Fernandez-de-Las-Penas, C., Madeleine, P., Arendt- Nielsen, L., 2008. Topographical mapping and mechanical pain sensitivity of myofascial trigger points in the infraspinatus muscle. Eur. J. Pain 12 (7), 859e865.
- Hillary A. Plummer, Jonathan C. Sum, Federico Pozzi, Rini Varghese, Lori A. Michener. Observational Scapular Dyskinesis: Known-Groups Validity in Patients With and Without Shoulder Pain. J Orthop Sports Phys Ther:1-25.
- Ibarra, J.M., Ge, H.Y., Wang, C., Martinez Vizcaino, V., Graven- Nielsen, T., Arendt-Nielsen, L., 2011. Latent myofascial trigger points are associated with an increased antagonistic muscle activity during agonist muscle contraction. J. Pain 12 (12), 1282e1288.
- Lucas KR, Polus BI, Rich PS. Latent myofascial trigger points: their effects on muscle activation and movement efficiency. J Bodyw Mov Ther. 2004;8:160-166Lucas KR, Polus BI, Rich PS. Latent myofascial trigger points: their effects on muscle activation and movement efficiency. J Bodyw Mov Ther. 2004;8:160-166
- Lucas KR, Polus BI, Rich PS. Latent myofascial trigger points: their effects on muscle activation and movement efficiency. J Bodyw Mov Ther. 2004;8:160-166Meininger, A.K., Figuerres, B.F., & Goldberg, B.A. (2011). Scapular winging: an update. The journal of The American Academy of Orthopaedic Surgeons, 19(8), 453-462.
- Simons, D.G., Travell, J.G., Simons, L.S., 1999. The Trigger Point Manual, Vol 1, 2nd Edition. Williams and Wilkins, Baltimore, USA.
- Wadsworth, D.J.S., Bullock-Saxton, J.E., 1997. Recruitment patterns of the scapular rotator muscles in freestyle swimmers with subacromial impingement. International Journal Sports Medicine 18, 618–624.