A common trend in orthopedics is to stop using the term “shoulder impingement” and start using the term “subacromial pain” instead.
Shoulder impingement is a really broad term that is used too often. It has become a commonly used junk term, such as “patellofemoral pain,” especially with physicians.
Other common variations include subacromial impingement or rotator cuff impingement, but it seems as if any pain originating from around the shoulder is often labeled as “shoulder impingement.”
Labeling “impingement” as a diagnosis may also be misleading. Impingement of the structures in your shoulder, such as the rotator cuff and bursae, also isn’t always a concern. In fact, every time you lift your arm, you technically “impinge” those structures.
You’ve done this every day for your entire life, so why does it hurt now?
Subacromial pain is probably an improvement over using the term impingement, but it’s still a vague term.
Unfortunately, the use of such a broad term as a diagnosis is not helpful to determine the treatment process. There is no magical “subacromial pain” or “shoulder impingement” protocol that you can pull out of your pocket and apply to a specific person.
I wish it were that simple.
This is also why conclusions are difficult to be drawn from meta-analyses and systematic reviews. A paper looking at hundreds of people aged 24-70+ with “shoulder pain” isn’t going to provide much clarity on what the best treatment options may be, it’s too diluted.
Luckily, a thorough subacromial pain examination can be used to determine the best treatment plan. Each person will likely present differently, which will require variations on how you approach their shoulder rehabilitation.
Most of the clinical examination for subacromial pain will still involve shoulder impingement provocative tests. Those are helpful, but the real challenge when working with someone with subacromial pain isn’t figuring out that they have shoulder pain, that’s fairly obvious. That’s why they are there.
It’s figuring out WHY they have shoulder pain, and what to do about it.
But before we get into that, let’s get this out of the way…
Is “Shoulder Impingement” a Bad Term?
A lot of people on social media think that we should stop using the term “shoulder impingement.” I’m not sure I feel that strongly about this.
Using any term to label or diagnose someone can be problematic. Maybe the question should be more about “how” we use it instead of “should” we use it. Is the problem really the “word” or is it the “message” that often goes with it?
I’ve personally used the term “shoulder impingement,” but for a very specific person for a very specific orthopedic concern.
As I previously mentioned above, every time you lift your arm you “impinge” your rotator cuff and bursae. There is contact between the soft tissue and boney structures.
I use “shoulder impingement” when this normally occurring impingement becomes symptomatic. To me, “shoulder impingement” should only be used for someone that has symptomatic impingement.
I also explain to people that impingement is normal, but that for some reason it has become symptomatic for them. This is likely due to their tissue capacity or a workload issue. You’ve tipped the scale and overloaded the tissue because your tissue wasn’t ready for the workload you applied to it.
Sure, I want to help them with their symptoms, but this now sets me up for what we really need to do – build capacity.
And just because an acromioplasty surgery does not provide better outcomes than physical therapy alone, this doesn’t mean that shoulder impingement is an inaccurate term. Maybe the selection criteria for those surgeries performed was poor? Acromioplasty has historically been a very commonly performed procedure for a variety of shoulder pain symptoms.
But more importantly, maybe treating the acromion isn’t treating the true issue, the imbalance between applied load and tissue capacity. Without addressing that, are we really going to solve anyone’s problem?
But we can’t also simply state that the shape of the acromion is irrelevant. Maybe it’s not as important as once hypothesized, but a gigantic hooked acromion that results in a smaller subacromial space is going to reduce the threshold of the capacity of the tissue. The threshold of normal impingement becoming symptomatic will be lower.
I think as a profession we can do better, but I think it’s more important that we clean up our “messaging” than simply change a term we use. “Words” don’t cause problems, “messages” do.
Simply changing the term to subacromial pain syndrome, rotator cuff disease, or many of the other proposed terms isn’t helpful to me. Heck, I’d rather be told I have shoulder impingement than a “syndrome” or “disease.”
Subacromial Pain: 3 Keys to Assessment and Treatment
To make the treatment process for subacromial pain a little more simple, there are 3 things that I typically consider to classify and differentiate shoulder impingement.
- The location of symptoms
- The structures involved
- The underlying cause of “shoulder impingement”
Each of these can significantly vary the treatment approach and how successful you are treating each person.
If you approach each patient with these 3 things in mind, you are going to do a much better job developing an effective treatment plan, versus just trying things and hoping they work.
I’ve called this the corrective exercise bell curve in the past. If you just throw the same treatments at every person with shoulder pain, you’ll probably get lucky 20% of the time, make them worse 20% of the time, and simply waste your time the rest.
Let’s dig in…
Location of Shoulder Impingement
The first thing to consider when evaluating someone with subacromial pain is the location of the impingement. This is generally in reference to the side of the rotator cuff where the impingement is located, either the outside of the rotator cuff or the undersurface of the rotator cuff.
These are broken down into either:
- Bursal-sided shoulder impingement – this is your traditional subacromial impingement
- Articular-sided shoulder impingement – this is called internal impingement
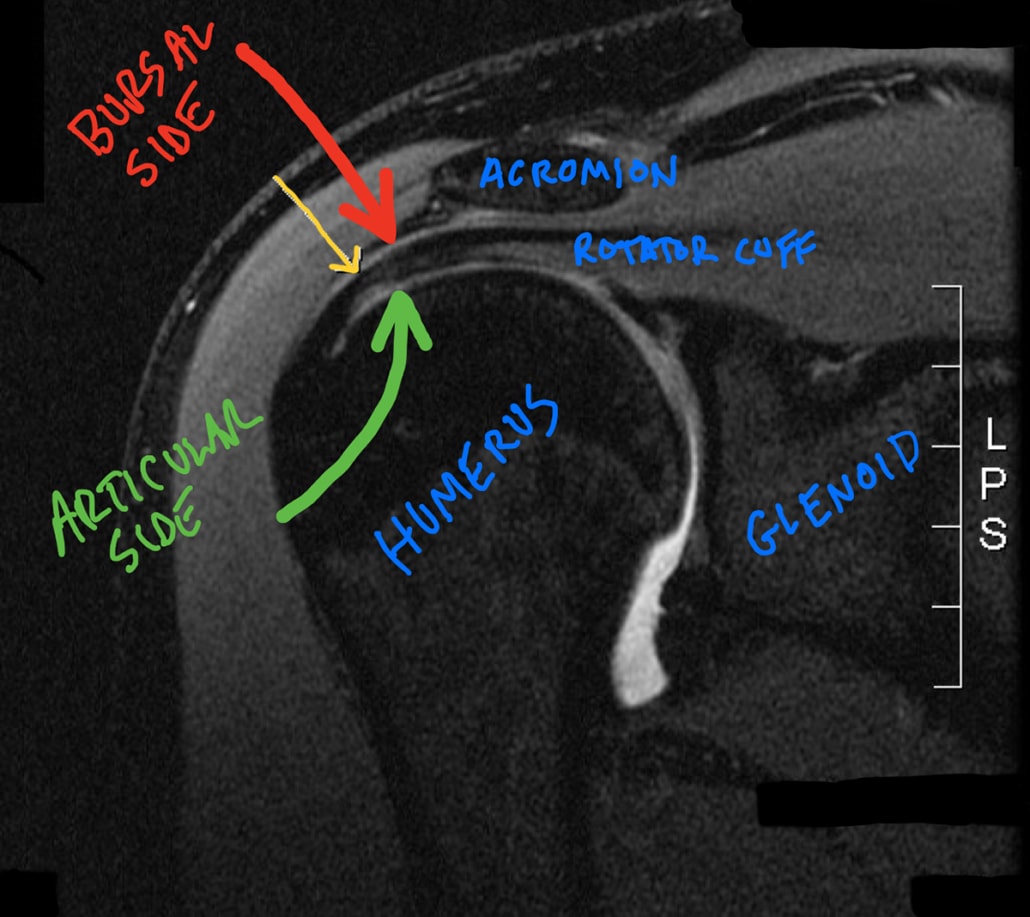
Bursal Sided Shoulder Impingement
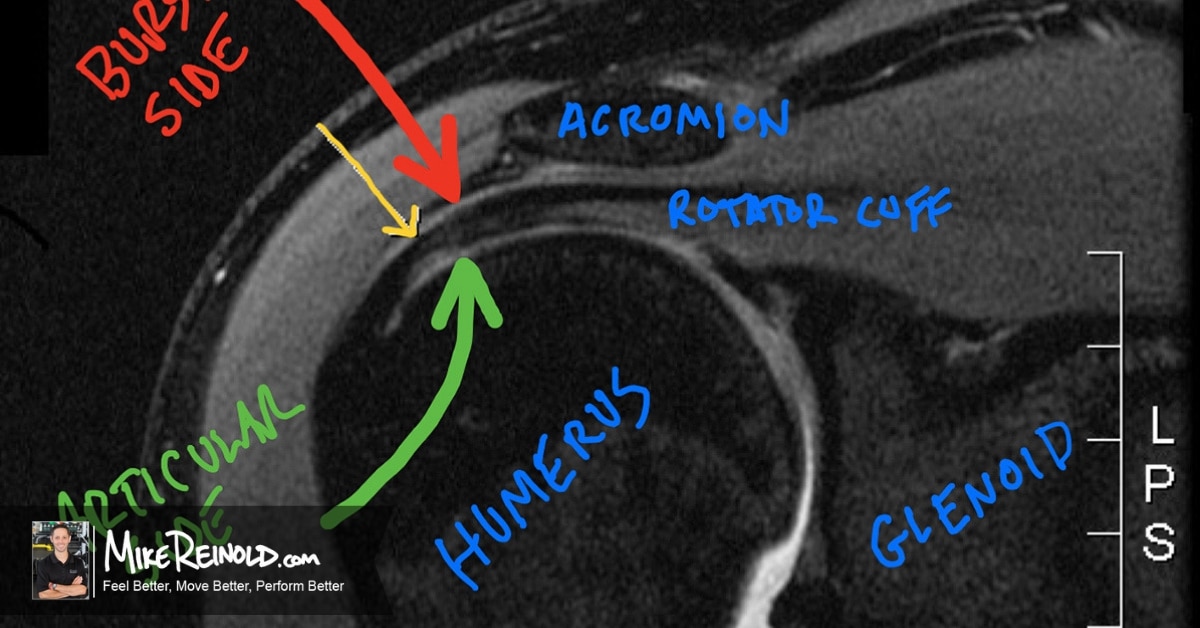
See the photo of a shoulder MRI above (photo credit). The bursal side is the outside of the rotator cuff, shown with the red arrow. This is probably your “standard” subacromial impingement that most people refer to when simply stating “shoulder impingement.”
This is often called subacromial impingement because the location of impingement occurs between the rotator cuff and the undersurface of the acromion, hence the term “subacromial.” This is also called the bursal side of the rotator cuff because there is a bursa located between the rotator cuff and the acromion, which acts as a shock absorber.
Articular Sided Shoulder Impingement
The green arrow shows the undersurface, or articular surface, of the rotator cuff. This Impingement on this side is often termed “internal impingement” because the impingement occurs on the inside, or joint side, of the rotator cuff. If you look closely at the image above, the yellow arrow shows an articular-sided partial-thickness rotator cuff tear. Note the irregularity of white at the bottom of the dark line of the rotator cuff.
This often involves the supraspinatus and infraspinatus rotator cuff muscles as the undersurface impinges against the glenoid joint rim. I’ll go over this in more detail below.
The two types of impingement are completely different and occur for different reasons, so this first distinction is important.
Because the cause of shoulder impingement is so different, the evaluation and treatment of subacromial and internal impingement will also be completely different. More about these later when we get into the evaluation and treatment.
Impinging Structures Involved
The next factor to discuss is which structures are involved. This is more for the bursal-sided, or subacromial impingement, and refers to what structure the rotator cuff is impinging against.
Take a look at the shoulder from the side view, with the front of the shoulder to the right and the back of the shoulder to the left. You can see the acromion is superior and the coracoid is a little more anterior. The coracoacromial ligament runs between these two areas.
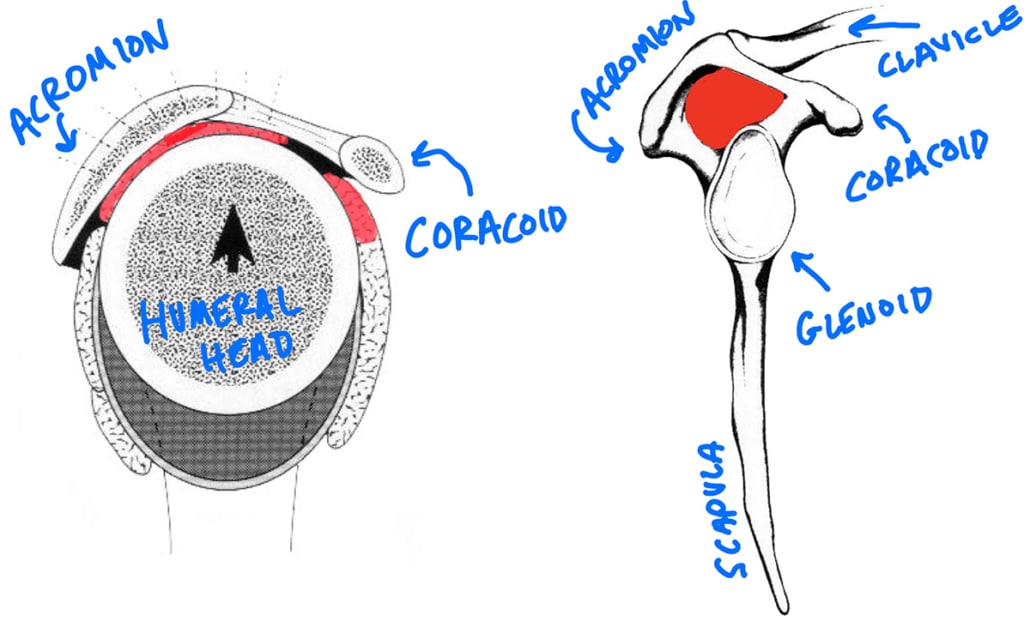
As you can see in the image, your subacromial space is pretty small (the red areas). It’s pretty easy to impinge on the acromion, coracoid, or coracoacromial arch. There isn’t a lot of room for error. In fact, this really isn’t a blank “space”, there are actually many structures running in this area including your rotator cuff and subacromial bursa.
Remember, you actually “impinge” every time you move your arm. We all do.
Impingement of these structures itself is normal and happens in all of us every time we use our arms. It’s when this becomes abnormal, excessive, or too frequent that shoulder pain and pathology occur.
This is why it is very shortsighted to say “impingement” is normal and that people should work through their discomfort. Yes, some impingement is normal, but excessive impingement is what may cause pain and pathology down the road.
So when it comes to the structures involved in impingement, I try to differentiate between subacromial and coracoacromial arch impingement. These can happen in combination or isolation and typically involve the supraspinatus rotator cuff muscle.
Another area that has received more attention lately is the subcoracoid space or the area below the coracoid. You can also have subcoracoid impingement. Because this is located more anteriorly, the subscapularis rotator cuff muscle can be involved with subcoracoid impingement.
The three types of bursal-sided impingement are fairly similar in regard to assessment and treatment, but I would make a couple of mild modifications for coracoacromial and subcoracoid impingement, which we will discuss below.
So if we were to get very specific, you can break shoulder impingement down into four different types based on the location and structures involved:
Bursal-sided impingement:
- Subacromial impingement – Involves the supraspinatus and acromion
- Coracoacromial impingement – Involves the supraspinatus and coracoacromial arch
- Subcoracoid impingement – Involves the subscapularis and coracoid
Articular-sided impingement:
- Internal impingement – Involves the supraspinatus and infraspinatus and glenoid rim
See what I mean? How can all of these be “shoulder impingement?” They all involved different muscles, different impinging structures, different locations, and different mechanisms!
OK, great, we now have differentiated and know “what” is impinging, we still don’t know “why” the person has impingement.
Cause of Shoulder Impingement
The next thing to look at is the actual reason why the person is experiencing subacromial pain.
Remember, I need to state this again, but “impingement” is normal. It’s when impingement becomes excessive or abnormal do we have symptoms. It’s less of an issue with the structures than it is with workload management.
There are two main classifications of causes that I refer to as “primary” or “secondary” shoulder impingement.
Primary Shoulder Impingement
Primary impingement means that the impingement is the main problem with the person.
A good example of this is someone that has impingement due to anatomical considerations, with a hooked tip of the acromion like this in the picture below. Many acromions are flat or curved, but some have a hook or even a spur attached to the tip (drawn in red):
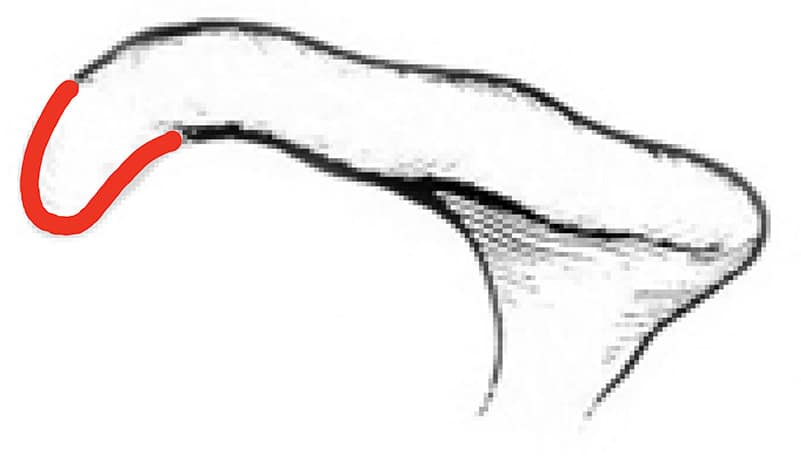
This also happens with the coracoid and subcoracoid impingement. An anatomical variation of the coracoid or bone spur can be present.
As our knowledge of shoulder impingement improves, it appears that the larger a bone spur, the more problematic it may become.
This is referred to as primary impingement because improving things like mobility, strength, and dynamic stability may be ineffective as there is a primary cause of impingement causing the symptoms.
Sure we may improve the symptoms and oftentimes are successful with rehabilitation, but sometimes we aren’t. It’s not because a certain treatment “isn’t effective for shoulder impingement.” It’s because there is a primary reason why impingement is occurring that we can’t change.
Without addressing the primary issue, like a large bone spur, working on secondary issues may not be effective.
Secondary Shoulder Impingement
Secondary impingement means that something else is causing impingement, perhaps their activities, posture, lack of dynamic stability, or muscle imbalances are causing the humeral head to shift in its center of rotation and cause impingement.
The most simple example of this is weakness of the rotator cuff.
The rotator cuff and larger muscle groups, like the deltoid, work together to move your arm in space.
The rotator cuff works to steer the ship by keeping the humeral head centered within the glenoid. The deltoid and larger muscles power the ship and move the arm.
Both muscles groups need to work together.
If rotator cuff weakness is present, the cuff may lose its ability to keep the humeral head centered. In this scenario, the deltoid will overpower the cuff and cause the humeral head to migrate superiorly, thus impinging the cuff between the humeral head and the acromion:
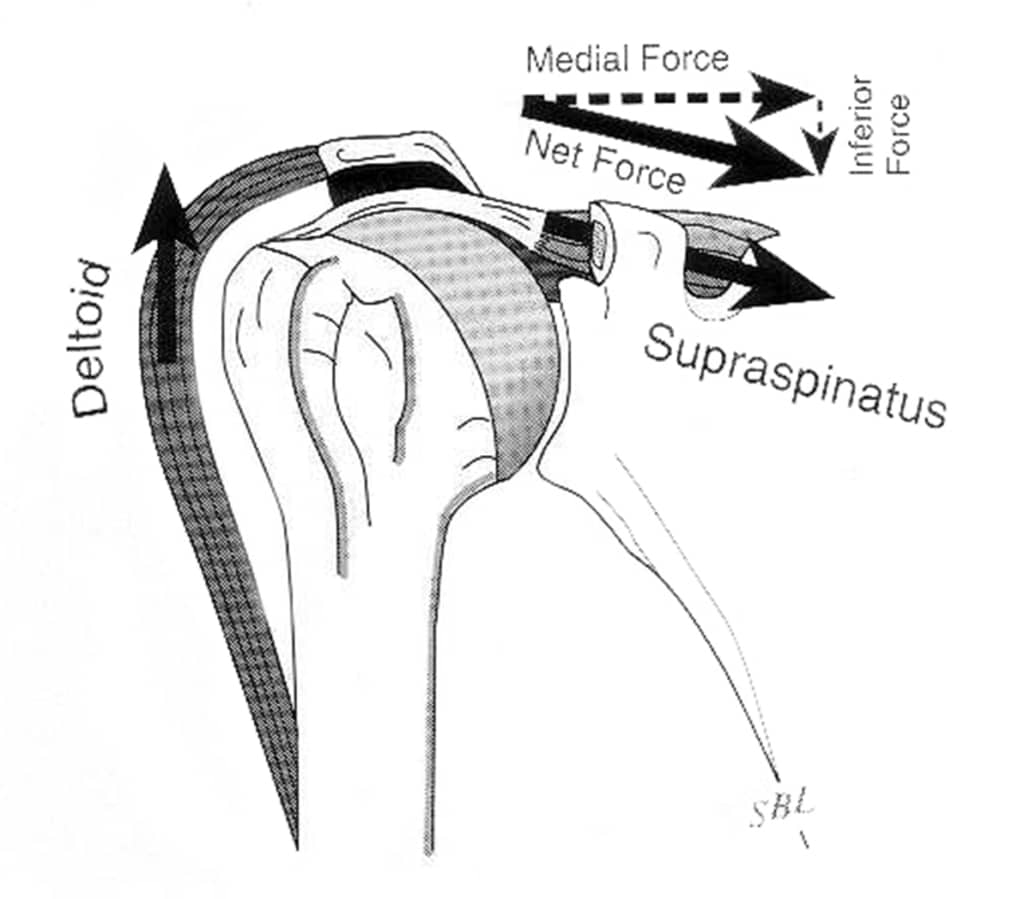
This is just a simple example, but as you can see is very impactful for shoulder function. It’s not just weakness of the rotator cuff, it’s also imbalanced strength ratios and improper timing of dynamic stabilization.
Other common reasons for secondary impingement include mobility restrictions and poor dynamic stability of the shoulder, scapula, and even the thoracic spine.
All of these areas need to work together to produce optimal shoulder function.
I see this a lot in my patients.
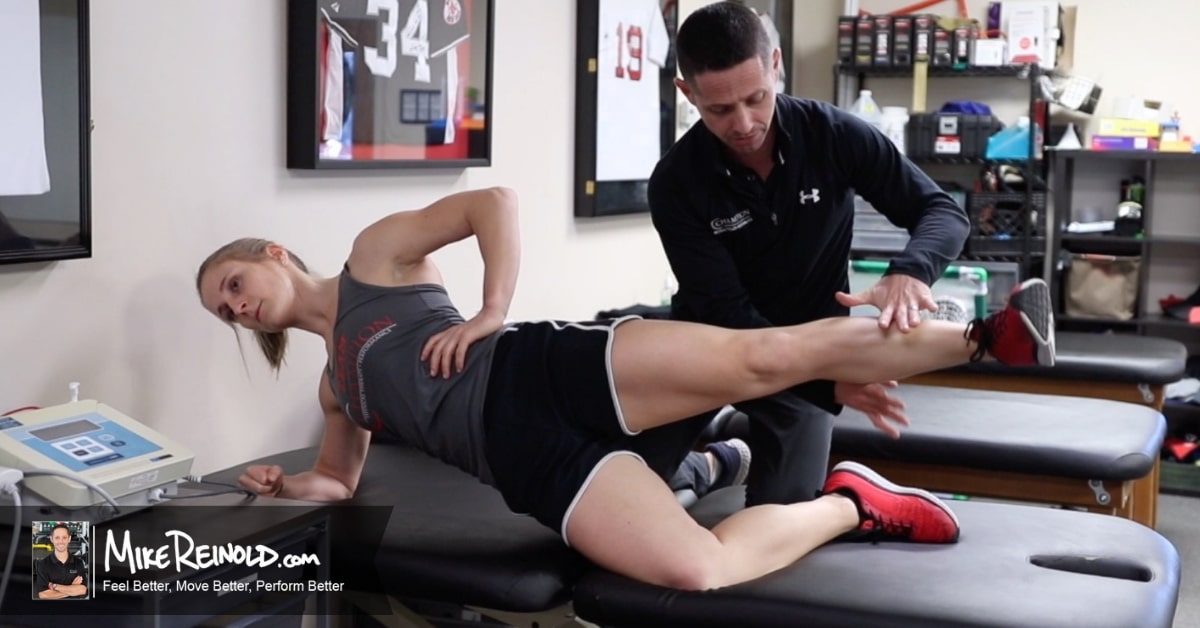
In the person below, you can see that they do not have full overhead mobility, yet they are trying to overhead press and other activities in the gym, flaring up their shoulder.
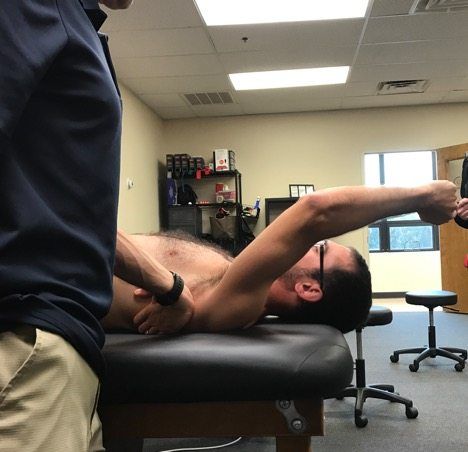
If all we did with this person was treat the location of the pain in his anterior shoulder, our success will be limited. He’ll return to the gym and start the process all over if we don’t restore this mobility restriction.
The funny thing about this is that people are rarely aware that they even have this limitation until you show them.
Also, keep in mind that this is not “chronic pain.” Sure this person has had shoulder pain for 8 months, but it’s because they keep irritating the area in the gym. This is more like recurring acute pain.
Understanding Tissue Capacity and Workload Management
One big topic I really want you to understand is symptomatic impingement can occur in people for completely different reasons based on their tissue capacity and workloads.
Compare these two people:
- A sedentary 55-year-old person who smokes, works a stressful desk job for 50+ hours a week, then comes home and just watches TV at night. They have not played a sport, exercised, or performed any manual labor for years.
- An active 26-year-old formal college football player that is now employed as a strength coach. Consistently trains for years and does a wide variety of recreational sports throughout the year.
If both of these people decided to do something out of the ordinary this weekend, like paint the walls and ceilings in a few rooms in their house, one of these people is more likely to overload their tissue capacity.
Guess which one?
It’s not fair to say “painting causes shoulder impingement.” But, you can see why it’s so hard to develop a research study that tries to correlate anything to symptoms.
Painting doesn’t cause impingement. Neither does smoking, or a sedentary lifestyle, or a hooked acromion, or rotator cuff weakness, or even posture and so many other things.
But…
Everything adds up and will impact the tissue’s capacity to manage a given workload.
Don’t get caught in the trap of saying that something doesn’t correlate in the literature with the development of shoulder impingement (or anything else). It is nearly impossible to determine this.
That doesn’t mean that focusing on rotator cuff strength or posture, as an example, is irrelevant. You still want to help build tissue capacity to handle workloads.
Special Tests for Shoulder Impingement
Another common theme on social media is that special tests for shoulder impingement are useless. This goes along with the theme that “impingement” is normal.
I think special tests for shoulder impingement are helpful.
There are a lot of things that can cause shoulder pain. I use special tests to try to help me determine what structures are involved. If someone had a labral tear, the special tests for shoulder impingement will likely not be painful, and vice versa.
And remember, I only consider using the term “shoulder impingent” when the movement is symptomatic. Even though we all impinge when we use our arms, special tests help me determine if that impingement produces symptoms.
Differentiating Between the Types of Shoulder Impingement
In my online shoulder program on the Evaluation and Treatment of the Shoulder, I talk about different ways to assess shoulder impingement that may impact your rehab or training. There are specific tests to assess each type of impingement we discussed above.
The two most popular special tests for shoulder impingement are the Neer test and the Hawkins test.
In the Neer test, the examiner stabilizes the scapula while passively elevating the shoulder, in effect impinging the humeral head into the acromion.
In the Hawkins test, the examiner elevates the arm to 90 degrees of abduction and forces the shoulder into internal rotation, impinging the cuff under the subacromial arch.
As I mentioned earlier, these special tests for shoulder impingement are provocative in nature, meaning that we are looking for the reproduction of pain.
Both of them will cause the structures to impinge in each of us, but they shouldn’t produce pain in a normal situation. But if the area is sensitive and irritable, it will cause pain.
You can alter these tests slightly to see if they elicit different symptoms that would be more indicative of the coracoacromial arch or subcoracoid types of subacromial impingement.
Because these structures are more anterior, we can alter the tests to better assess this area.
The Neer test can be performed in the sagittal plane, and the Hawkins test can be modified and performed in a more horizontally adducted position. Both of these positions will impinge more anteriorly.

There is a good chance that many patients with subacromial pain may be symptomatic with all of the above tests, but you may be able to detect the location of subacromial impingement (acromial versus coracoacromial arch) by watching for subtle changes in symptoms with the above four tests.
Now, before we go any further, let’s talk briefly about the reported accuracy of these tests in the literature.
Just like we’ve talked about with the studies looking at the treatment effectiveness in people with shoulder impingement, most studies published vaguely look at how accurate a test may be at detecting “impingement.” Hopefully, if you’ve gotten this far in the article, you see how flawed this approach is, as this is simply too broad.
How can we evaluate how “specific” a special test is for such a “non-specific” diagnosis?
Internal impingement is a different beast.
This type of impingement, which is most commonly seen in overhead athletes, is typically the result of some hyperlaxity of the shoulder in the anterior direction.
As the athlete comes into full external rotation, such as the position of a baseball pitch, tennis serve, volleyball serve, and others, the humeral head slides anterior slightly causing the undersurface of the cuff to impinge on the inside against the posterior-superior glenoid rim and labrum.
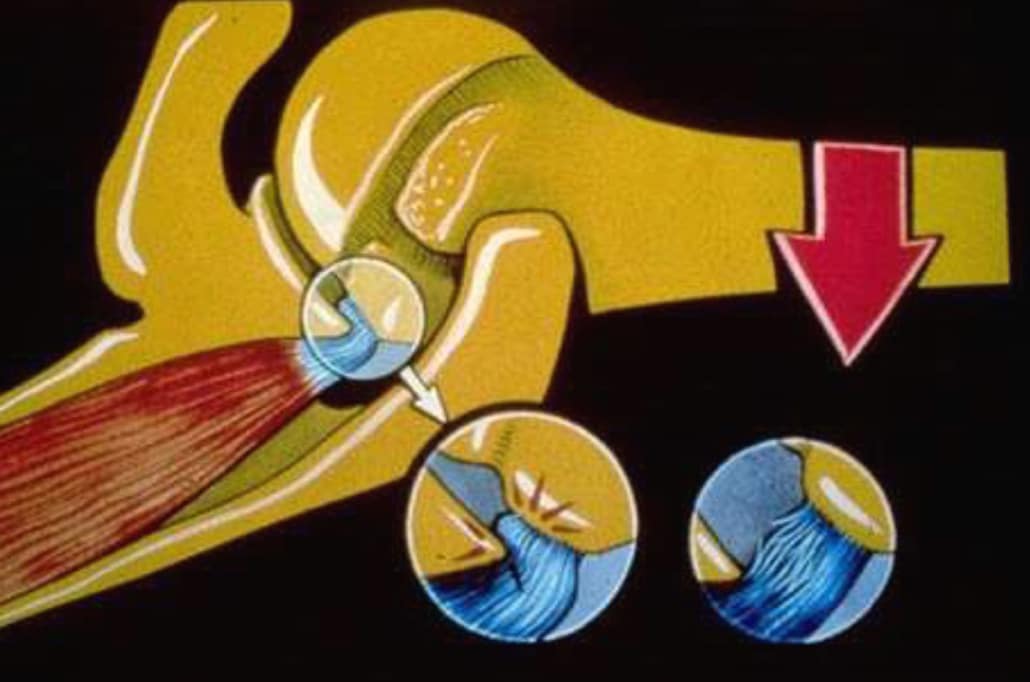
This is what you hear of when baseball players have “partial-thickness rotator cuff tears” the majority of the time. They aren’t the same partial-thickness tears your grandmother has.
The best special test for internal impingement is simple and is exactly the same as an anterior apprehension test.
The examiner externally rotates the arm at 90 degrees abduction and watches for symptoms. Unlike the shoulder instability patient, someone with internal impingement will not feel apprehension or anterior symptoms. Rather, they will have a very specific point of tenderness in the posterosuperior aspect of the shoulder. When the examiner relocates the shoulder by giving a slight posterior glide of the humeral head, the posterosuperior pain diminishes.
3 Keys to Treating Subacromial Pain – How Does Treatment Vary?
Using the three main keys from the above information, you can alter your treatment and training programs based on the specifics exhibited:
- The location of shoulder impingement – bursal- or articular-sided impingement
- The structures involved – Subacromial, coracoacromial arch, subcoracoid, or internal impingement
- The underlying cause of shoulder impingement – primary or secondary.
I promise you are going to have much more success in designing a physical therapy or training program if you factor in these keys.
Treating Different Types of Subacromial Pain
As I hope you can now see, to properly treat subacromila pain you should differentiate between subacromial, coracoacromial, subcoracoid, and internal impingement.
Treatment is similar between these types of impingement. There is a bunch of overlap.
However, there are some differences:
- With subacromial impingement, you should be cautious with overhead activities that produce discomfort
- With the more anterior-based coracoacromial arch and subcoracoid impingement, you need to be cautious with elevation in more of a sagittal plane and horizontal adduction movements that produce discomfort
- With internal impingement, you should be cautious with excessive external rotation at 90 degrees abduction (like the throwing position) that produce discomfort
Notice that I said “that produces discomfort” for all three? The key here for me is that you should not work through discomfort or a “pinch” with impingement.
A “pinch” is the impingement of a sensitive structure!
I’m not a fan of working through pain with shoulder impingement. That shows me that you either have a primary or secondary cause of impingement that hasn’t been addressed. Trying to work through this could actually just irritate it more.
You can build capacity in an area that does not cause symptoms, then slowly progress.
Treating Primary Versus Secondary Shoulder Impingement
This is an important one and often a source of frustration for young clinicians.
If you are dealing with secondary impingement, you can treat the person’s symptoms all you want, but they will come back if you do not address the underlying reason why they have symptoms.
Again, this is probably why acromioplasty surgery doesn’t seem to be very effective in isolation.
But please remember, I do treat their symptoms because that is why they came to see me.
I want to reduce symptoms. This is going to allow me to do more in the long term. However, this should not be the primary focus if you want long-term success.
This is where a more global look at the patient, their posture, muscle imbalances, and movement patterns all come into play. Then, helping to build capacity by loading the tissue in an intelligently designed progression.
Breakthrough and see patients in this light and you will see much better outcomes.
You should have a systemized way of assessing movement and building programs to optimize and enhance their function. If you don’t you really should check out my system in my free online Introduction to Performance Therapy and Training course.
A good discussion of the activities that are causing their symptoms may also shed some light on why they are having shoulder pain.
Again, using the example above, if you don’t have full mobility and try to force the shoulder through this motion restriction you are going to likely cause some irritation.
This is especially true if you add speed, loading, and repetition, such as during many exercises in the gym.
I spend a great deal of time discussing what “zones” of motion the person should be working in. Essentially, I try to develop a “green zone” and a “red zone” depending on when they have symptoms.

It’s important to continue working within their green zone and not simply say “take a few weeks off.” And slowly over time, our goal is to expand their green zone and reduce their red zone.
Treating Internal Impingement
Internal impingement involves a little more discussion. The main thing to realize with internal impingement is that this is pretty much a secondary issue. It is going to occur with any cuff weakness, fatigue, or loss of the ability to dynamically stabilize.
The overhead athlete will show some hyperlaxity in the “lay back” shoulder position of external rotation. Most overhead athletes have underlying laxity, what tends to happen is they lose strength or have an excessive workload that causes fatigue, and then the structures impingement more and become irritable.
Treat the cuff weakness and its ability to dynamically stabilize to relieve the impingement. This often includes an initial period of rest and then building back their strength and dynamic stability.
How to treat internal impingement is a huge topic that I cover in a webinar for my Inner Circle members.
Learn Exactly How I Evaluate and Treat the Shoulder
If you thought this article was helpful and are interested in mastering your understanding of the shoulder, I have my acclaiming online program that will teach you exactly how I evaluate and treat the shoulder.
The online program takes you through everything you need to become a shoulder expert. You can learn at your own pace in the comfort of your own home. In addition to shoulder impingement, you’ll learn about:
- The evaluation of the shoulder
- Selecting exercises for the shoulder
- Manual resistance and dynamic stabilization drills for the shoulder
- Nonoperative and postoperative rehabilitation
- Rotator cuff injuries
- Shoulder instability
- SLAP lesions
- The stiff shoulder
- Manual therapy for the shoulder
The program offers CEU hours for physical therapists and athletic trainers. Click below to learn more: