I will admit something that may surprise you: Corrective exercises don’t always work for me. There, I said it. I feel liberated now!
Corrective exercises have become popular in the rehab world and probably even more so in the fitness world. Everyone is now assessing biomechanics and movement patterns and trying to prescribe corrective exercises to address what they see.
This is fantastic.
I recently co-authored an article with Jon Goodman from the Personal Trainer Development Center on how physical therapy and personal training can collaborate more effectively. We discussed this concept briefly.
Jon took a more hard stance against personal trainers performing assessments for several reasons that he discussed. I don’t feel as strongly as Jon on the subject and welcome the development of systems like the Functional Movement Screen that all of us can use to examine movement patterns and communicate better between professions.
Anything we can do to individualize someone’s programming is awesome in my mind.
But there is a caveat…
There is a dirty little secret that I don’t hear a lot of people talking about – corrective exercises don’t always work.
This has almost become like the story of the Emperor’s New Clothes, where people are a little afraid to admit that corrective exercises don’t always work. Perhaps they think they aren’t skilled or intelligent enough to make the corrective exercises work!
Well, I am here to make you feel better. Corrective exercises don’t always work for me, and understanding why they “don’t work” is just as crucial to understanding why they “do work.”
The Corrective Exercise Bell Curve
I have developed the corrective exercise bell curve to better illustrate the spectrum of corrective exercise efficacy.
The bell curve explains why some people don’t respond to corrective exercises. I am not 100% certain of the exact percentages; this is just a model, but it is a starting point for discussion, at least.
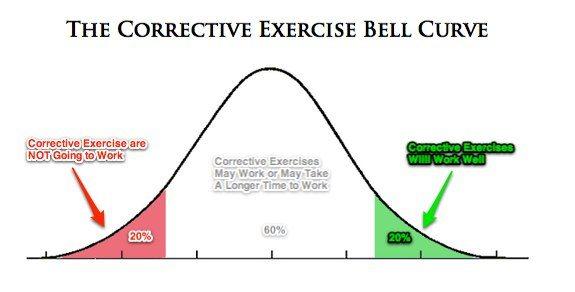
In this diagram, you can see that a certain percentage of people will respond very favorably (and often rapidly) to corrective exercise. These are the all-stars that we all love to work with—call them the rapid responders!
Conversely, there is a certain percentage of people who just won’t respond to corrective exercises at all. For these people, something is preventing the correctives from working. Perhaps it is pain, pathology, biomechanical issues, structural abnormalities, or even neurological.
These people essentially need more than corrective exercises.
Then, there is everyone else in the middle. These are the people who may respond to a few corrective exercises, but it probably isn’t going to be a quick fix. They are going to take some time and often feel like they aren’t making progress.
Applying the Corrective Exercise Bell Curve
This is all important to understand so you can begin to classify the people you screen. If you are a fitness professional who just performed a movement screen, programmed some corrective exercises, and was able to clean up some poor movement patterns, congratulations! That is awesome, you did a great job for your client and maybe even saved our healthcare system some money in the future!
I really see the benefit of collaborating between personal trainers and physical therapists for people who do not respond to corrective exercises.
We can do much greater things together than alone!
For the smaller percentage that will never respond to corrective exercises alone, they need a full physical therapy evaluation and a combination of treatments, including manual therapy techniques, neuromuscular motor planning techniques, and eventually corrective exercises.
But here is the really cool group to work with—everyone else! This is the gray area where we could really collaborate well to help people achieve their goals. Notice that in the middle group, I stated that corrective exercises may work or may take longer to work. In this situation, if physical therapists and personal trainers collaborated more, we could really make a difference in a lot of people.
Physical therapy can work in tandem with personal training to help people achieve their goals faster by combining manual therapy with workouts.
I’m lucky. Throughout my career, I have worked side by side with some of the best strength coaches and personal trainers, people who have made me better at what I do. This is by far my ideal work environment, and that’s why I always try to team up with a multidisciplinary group of people.
Examples
Let me come up with a couple of examples to illustrate better. Perhaps you notice someone with pretty poor squat mechanics. Corrective exercises aren’t working. This is a perfect person for a physical therapist to collaborate with.
Perhaps their hip is tight (this is just an example; it could be several things). All they may need is a kickstart in the right direction with specific manual therapy, and they may be good to go.
Or how about you screen someone with really poor shoulder mobility on one side? They don’t really have many symptoms other than a general ache in their shoulder from time to time, but the corrective exercises don’t seem to be working.
I was actually referred a patient just like this last week from one of the personal trainers I work with frequently. That specific patient had very specific glenohumeral capsular tightness that wouldn’t improve with corrective exercises alone.
I do this all the time and can often clean up someone’s patterns in a few sessions, sometimes even less, by using the proper manual therapy techniques in addition to exercise to address their concerns while they continue to train. To me, that is fun—helping people achieve their goals faster through collaboration.
So next time you feel like your corrective exercises are not working, don’t feel bad about it. You are not alone. If you are a physical therapist or personal trainer, find a respective partner to collaborate with and remember the corrective exercise bell curve.




