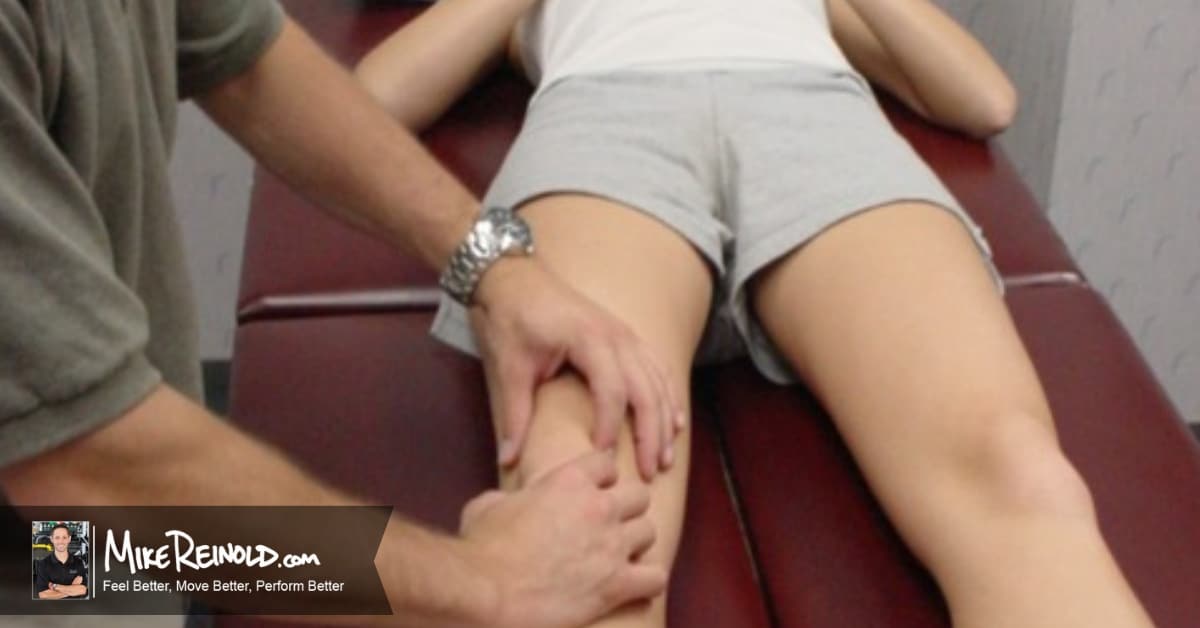
Measuring the position and mobility of the patella is still a very important component of my clinical examination of the knee. It gives me a great sense of soft tissue restrictions that may be present when patellar hypomobility is noted. This is especially common after knee surgery. But measuring patella mobility is also important to assess generalized laxity when patellar hypermobility is observed.
The first time you feel either of these during your clinical exam, you’ll know what I mean.
But if you read through the literature, you may find conflicting results regarding the validity and reliability of assessing patella position and mobility.
The Reliability of Measuring Patella Mobility
One study that I reference often is a systematic review by Smith, who looked at the reliability of assessing patella position, specifically in the medial-lateral position. Like any examination technique that is commonly performed, it is necessary to establish that the test has adequate intra-rater and inter-rater reliability. The test needs to be easily replicated and produce accurate results both between two different clinicians but also when repeated during re-evaluation with the same clinician.
Otherwise, the test may have limited use and not be able to provide helpful information.
The authors conclude the intra-tester reliability is good to assess medial-lateral patellar position, but inter-tester reliability was variable. The variability is interesting to me and makes me wonder if we just aren’t standardizing how we look at patella mobility.
Another study by Herrington demonstrated that a group of 20 experienced therapists could reliably measure patellar position. This tells me that a group of similar trained or skilled clinicians will show greater inter-tester reliability than a randomized selection of clinicians. When I see that a test has good intra-tester and worse inter-tester reliability, I think one of two things:
The test is difficult to perform and/or is more accurate with more experience.
Reliability can be enhanced if we all use the same examination techniques. There may be subtle differences in techniques that may produce poor inter-tester reliability. This is what came to my mind when the Herrington study showed good inter-tester reliability with a group of experienced clinicians.
The Validity of Measuring Patella Mobility
In regard to validity of the measurements, the authors conclude that the criterion validity of this test is at worse moderate, based on limited evidence. However, a couple of interesting studies were referenced. A study by McEwan demonstrated that a lateral tilt of the patella greater than 5 degrees can be detected. This was confirmed with MRI measurements. The previously reported study by Herrington also reported that medial-lateral patellar position could accurately be measured as confirmed by MRI measurements.
A Simple Way to Measure Patella Mobility
It appears that clinical measurements of patellar positions can be both reliable and valid. While intra-tester reliability, or your own ability to accurately repeat a test, appears to be more accurate, inter-tester reliability may be enhanced with a standardized examination technique.
Taking all this into consideration, I honestly do not try to “measure” patellar position.
I will assess the position but I do not try to place a label, such as millimeters or degrees, on the exact position. If I want or need this information, I would much rather obtain this from a MRI. I focus more on assessing the amount of hypomobility or hypermobility.
And there is a really simple way that we can do this that I think will great enhance our reliability.
To simplify this measurement, I try to just use a percentage of the patella that I feel can displace. Here is how I do it:
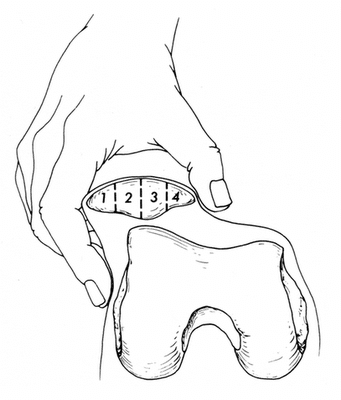
- I break the patella down into 4 equal segments representing 25% of the width of the patella each.
- I visually try to establish where I believe the midline of the trochlea is located when I am measuring position. If I am measuring displacement, I will visualize the edge of the lateral trochlea.
- I then measure the percentage of the patella that is positioned beyond the midline of the trochlea and then displace the patella and attempt to determine if 25%, 50%, 75%, or 100% of the patella can displace beyond the lateral edge of the trochlea, as in the image below:
I’ve learned over the years that knee experts, such as Dr. Frank Noyes, consider 50% displacement to be “normal.” I use that as a frame of reference, but comparing side-to-side is probably even more important.
I feel that this provides me with plenty of information to compare to the other extremity and simplifies the process, which I hope would enhance intra- and inter-tester reliability. If we all do it this way, I think we’ll be far more accurate.
What do you think? Is this too simple? How do you measure patellar mobility?