Today’s post on returning to exercise after COVID-19 is a great guest article from Alex Hubelbank. Alex is a strength coach, athletic trainer, physical therapy student, and competitive powerlifter. Unfortunately, Alex was diagnosed with COVID several weeks ago. She’s currently doing well, but as she navigates her own personal return to exercise, she wanted to share what she has learned and experienced to help others. *** All of the medical recommendations in this post are supported by current literature in COVID-19 management. We do not claim to be the best resource, but instead, she is simply using her understanding to synthesize the research and educate her peers. All COVID-19 patients should consult their medical provider for more specific recommendations. Click here to read the most up to date information from the CDC website.***
Over the past week, I have found myself with a bit more time, as my DPT semester has wrapped up and I tested positive for COVID-19. By the CDC recommendation, I am isolating at home and hoping my symptoms resolve quickly.
With this forced rest, I have spent more time out of the gym than I am accustomed to, being that training is such a significant part of my life personally and professionally.
As I start to feel better, I began to do some research on when it may be safe to return to my usual training regimen, especially with much of the media information suggesting it could be a while.
What I found through my research as a Strength & Conditioning coach, Athletic Trainer and current DPT student made me dive deeper and try to “science” my way into a safe, appropriate return to activity plan.
The purpose of this post is to synthesize the currently available literature regarding the return to exercise and activity after a mild (non-hospitalized) case of COVID-19 in an otherwise healthy population. We tend to believe we are invincible to the perils of the coronavirus and I can assure you, we are not.
Here’s what I have learned and how I plan to return back to exercise based on all the information I could find.
How COVID Impacts the Body
For a better understanding, I will explain COVID-19 in an overly simple way based on what is currently believed in the medical community. As our understanding of COVID continues to evolve, I urge you to stay current with CDC recommendations.
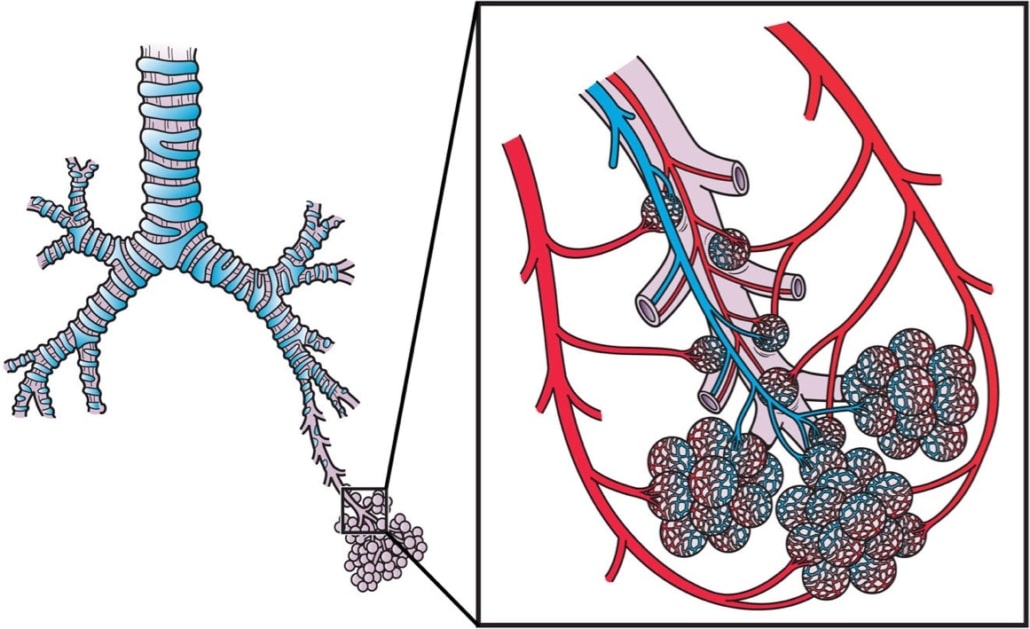
SARS-CoV-2 (COVID-19) is mainly transmitted through respiratory droplets and close personal contacts. The virus is believed to enter the body primarily through the nose where it replicates and spreads down the respiratory tract to the lungs as well as many other parts of the body.
The virus then is taken up by macrophages in the lungs responsible for clearing foreign bodies. The virus causes damage to the grapelike structures at the bottom of your lungs (alveoli), which are primarily responsible for trading oxygen from the air inhaled with your bloodstream to circulate it to your body.
This decrease in the body’s ability to distribute oxygen can have severe implications even in mild cases. This is known as a ventilation/ perfusion (V/P) mismatch, where the air is getting into the lungs effectively (ventilation), but the oxygen trade is not working as it normally would (perfusion).
The effects of COVID have been observed throughout the body, with documented impact on the cardiac, pulmonary, hematologic, musculoskeletal, gastrointestinal systems, neurological, psychological, dermatological, and renal systems.
In addition to continued breathing difficulties, some patients (including many reported cases in elite athletes and otherwise healthy people) experience extreme fatigue, irregular heart rhythms, inflammation of the heart muscle (myocarditis), muscle aches, gastrointestinal upset, and blood clots.
While your physical fitness may help dampen your COVID-19 case, it does not exempt you from developing one of these.
One study in JAMA Cardiology looked at 100 men and women in Germany, average age 49, who had recovered from Covid-19, and found signs of myocarditis (an inflammatory condition of the heart) in 78 percent. Most had been healthy, with no pre-existing medical conditions, before becoming infected.
More than a dozen women on the U.S. Olympic rowing team who contracted the virus in March described persistent fatigue for weeks after the initial illness.
It is important to understand some of the primary complications of COVID that may complicate your return to exercise.
Myocarditis and Heart Arrhythmias
It has been suggested that this is caused by inflammation overload triggered by the virus, which can cause arrhythmias or heart inflammation. Symptoms include extreme shortness of breath out of proportion to the activity you are doing, racing or irregular heartbeat, chest tightness, lightheadedness, or passing out.
In a recent study of 26 male and female college athletes, previously healthy, with mild or asymptomatic COVID-19 cases, 15% displayed symptoms of myocarditis which can result in cardiac arrest and possible death in overexertion.
Acute Respiratory Distress Syndrome
Relating to the oxygen trade mentioned earlier, this depleted exchange can become so severe that your body is no longer receiving adequate oxygen which becomes a medical emergency. While not common in mild cases, it has been reported. Symptoms here are shortness of breath, blue tint to the skin (indicating a lack of oxygen), oxygen saturation below 93% (can be measured at home with a pulse oximeter).
Venothromboembolism (VTE)
This is referring to blood clots in the extremities that can mobilize to the lungs and become a medical emergency. It is not currently understood why this occurs, but even in mild cases, it is a risk worth noting. Symptoms include leg pain on both sides that does not seem to be associated with an activity, tightness in the calves, among others. Mobility can improve the risk of developing VTE.
Returning to Exercise After COVID
In recent years, “sitting” has been dubbed as the new “smoking,” or as Mike Reinold likes to say, “not moving is the new smoking.” so in the active population, it is unbelievably challenging to keep us from our regular fitness routine! Physical inactivity is a widely recognized risk to physical and mental health associated with increased all-cause mortality. A 2-week reduction in daily steps from 10,000 to 1500 steps has been shown to impair insulin sensitivity and lipid metabolism and increase visceral fat in otherwise healthy adults.
But we need to be cautious when returning back to exercise after COVID.
There have been more than a handful of cases of previously young healthy patients with mild COVID presentations feeling well enough to exercise, who have returned to exercise too early and experienced difficulty or worsening symptoms.
Most simply didn’t know that COVID-19 had still been impacting their system, coupled with the strain of exercise, and attempted to return to activity too soon.
When I began my research, I was under the impression I could follow the frequently used “neck check” recommendation for exercise after a standard virus, suggesting that if my symptoms were from the neck up, I was in the clear.
I quickly learned that due to COVID-19’s multisystem impact, this is not sufficient. The areas of primary concern are cardiac (myocarditis, arrhythmias), pulmonary (lungs), and vascular (blood clots). All of which are essential and heavily influenced by vitality and exercise.
Luckily, I am here to tell you that there is a way to return to fitness safely.
With the help of your PCP and the recommendations below, you can be vigilant to your condition and combat the risks of adopting a sedentary life. The Hospital For Special Surgery was the first institution to make recommendations for the aforementioned population to return to exercise and I have done my best to communicate them below.
HSS Considerations for Returning to Exercise After COVID
- Each patient with COVID-19 is unique. Although general patterns in COVID-19 have been reported, there is a wide variance of disease expression.
- Each patient with COVID-19 recovers at a unique rate. There is currently no algorithm guiding a patient’s stepwise return to activity.
- The severity of the disease appears to affect the duration of recovery, although this has yet to be proven.
- Return to activity after COVID-19 should be guided by a body-system approach that includes the cardiac, pulmonary, hematologic, musculoskeletal, and gastrointestinal systems.
- Clinicians should advise patients to return to activity in a slow, gradual, stepwise manner.
- Patients should be given instructions to speak with their health care provider should they develop symptoms in the body systems listed above.
HSS Recommendations for Returning to Exercise After COVID
- Exercise should not resume if a patient with COVID-19 has a persistent fever, dyspnea at rest, cough, chest pain, or palpitations.
- Any COVID-19 patient with an underlying cardiovascular or pulmonary condition should consult a physician prior to the resumption of exercise, even if asymptomatic.
- An otherwise healthy patient with a self-limited course of COVID-19 who has been asymptomatic for 7 days may begin resuming physical activity at 50% of normal intensity and volume.
- Consultation with a physician is recommended if patients who have had COVID-19 develop chest pain, fever, palpitations, or dyspnea on the resumption of exercise.
My Plan to Return to Exercise Following COVID-19

While these recommendations are helpful, it can be overwhelming to understand where exactly to start.
Here is where I put on my thinking cap to create further recommendations within the parameters from the experts and my understanding of physiology.
Between HSS and other international organizations who have reported on safe return to activity, the average is 10 days from symptom presentation AND 7 days from symptom resolution to begin progressing exercise.
The authors of this guideline from HSS suggest that with mild symptoms, consider limiting activity to < or = 3 METS or equivalent (walking at a 3mph pace) while also limiting sedentary periods. One MET roughly correlates with an 8-12 beats per minute increase in heart rate. Additionally, at least one week of light stretching and muscle strengthening activity should be tried prior to beginning cardiovascular sessions.
This may feel backward, but as we now know, COVID-19 is primarily considered a respiratory condition, so beginning to reintegrate exercise without taxing the cardiovascular system can be a more beneficial approach, leading to better progression of activity. Splitting these sessions into shorter bouts can aid in reducing fatigue, risk of clots, and shortness of breath by lowering the intensity.
As of right now, I am awaiting an appointment with my physician to follow up on my COVID-19 diagnosis and discuss the battery of tests that may be appropriate to clear me for exercise. My remaining symptoms are occasional confusion, mild headache upon exertion, 80% loss of smell and taste, as well as minor chest pain.
I am fourteen days from symptom presentation. As I await full clearance from my PCP, I have begun to ramp up my activity through creative options. I am doing daily light yoga through Youtube, taking at least three walks per day, have done a few bodyweight circuits with the intent only to finish it. I am learning more patience with myself not to become frustrated that I can barely bench press twenty-five pounds, an 85% decrease from my usual abilities. I am focusing on the elements I can control like sleep, hydration, stress management, and taking each day to get a little bit better.
How to Track Progress
Once I get going with my exercise, I am going to follow the below guidelines to monitor my progress:
- Heart rate: Should increase linearly with activity. If it doesn’t follow this pattern, I’ll slow down and see what happens. If I experience palpitations, I will stop and consult my physician.
- Respiratory Rate: Should also increase steadily, if I’m feeling abnormally short of breath, I’ll stop and consult my physician.
- Pulse Oximetry: this should remain the same or increase with activity; if it drops to 93% or less; stop, recheck, and consult my doctor if it does not improve.
- Listen to My body: this is going to be slower than I think, I will let my body tell me when I’m ready to progress.
My Exercise Plan
As I begin my own journey back to fitness, I wanted to share where I was before and what some options I have considered to stay somewhat active within my current limitations to minimize the effects of being sedentary.
My typical training pre-COVID-19 was 4-5 days a week of high intensity strength training, plus 2-4 days a week of aerobic conditioning.
At this point on in the process my options for activity each day include:
- 3 20-minute walks/ day @ 20-24 minute mile pace (typically 17 minute pace).
- Some days alternating with 10-15 minute spin bike ride (monitoring pulse ox during ride) at a comfortable pace (I could have a conversation while pedaling).
- 20 minute light yoga
- Walk the stairs in the house a few times and assess vital signs (heart rate, pulse ox, skin color)
- Break up the workout. If you typically do an hour, start with 30 minutes (potentially even split into two 15-minute sessions) and build up based on how you respond.
As I start to feel better I am going to start the following strength training progression:
- 3-4 exercise circuit at low-moderate intensity with 1-2 minutes rest between rounds (at home)
- Push Ups
- Goblet Squat
- Bicep Curls
- Side Plank
- Split Squats
- When returning to the gym:
- Dumbbell/ machine only to start – taking a page out of bodybuilding and focusing on isolation exercises to minimize cardiovascular load.
Overall, my hope is that this has given you enough to begin your process. I know it can be frustrating and difficult not to go right back to where you were before! I don’t know how long it will take, but I do know that I will get there and so will you.
Most importantly, I hope that you have been encouraged to work with your doctor to find the right solution for you!
Once you have been cleared, use these recommendations to guide you. If you do not feel comfortable navigating exercise alone, consult with a trusted trainer, coach, or physical therapist to identify the best solution. Let’s science our way back to health!
5 Week Update
I took me ~35 days after getting COVID before I finished a whole week of training. While I felt mostly normal, there were several things I noticed
Taste and smell weren’t fully recovered. I kept catching myself flavoring things a lot more, adding calories or salt to my meals. Caffeine consumption caused an abnormal HR response than usual for me.
Since powerlifting requires Valsalva at some points, that had been a big limiter (having to use lighter weights and short sets which isn’t usually how I train) because of how high my heart rate would spike.
I’m still exhausted after training, and overall more fatigued in general. I’ve been requiring 8-9 hours of sleep, which is more than usual for me.
I also still feel like I’m having some periods of mental confusion.
Oh, and one weird one… I feel like my sneezes are bigger!
Luckily, I’m meticulous about tracking my health. I use an Apple Watch and Whoop to measure data. Pre-COVID versus 5-weeks post:
| Pre-COVID | 5 Weeks Post COVID | |
| Resting Heart Rate | 52 bpm | 62 bpm |
| Nocturnal Respiratory Rate | 14 breaths / min | 15.5 breaths / min |
| Total Tonnage Lifted Squat Training % Bench Training % Deadlift Training % | 73,490 lbs 80% 2×2 92.5% 2×2 80% 3×3 | 41,800 lbs 55% 3×5 75% 2×4 70% 5×3 |
As you can see, my training capacity is much lower with a > 50% reduction in tonnage lifted. Prior to COVID I was strength training 5 days per week, along with 1 conditioning day, and 2-3 walks per week. As I ramped training back up, I was doing a lot more walking to get some activity while I was unable to exercise at a high intensity. I had moved to 4 days strength training and 3-5 walks per week.
8 Week Update
At 8 weeks out from COVID-19 I finanly felt that my training had gone back to normal. I’m back up to 5 days a week of powerlifting style training and a few walks here and there.
I received the Moderna vaccine on January 28th and was totally down for the count on the 29th. I was surprised that the shot itself was less painful than a flu shot, but I felt identical to the first day of COVID symptoms for an entire 24 hours. Fevers, chills, body aches, and a headache. On the 30th, I woke up and the only reminder of the vaccine was a slightly sore arm.
My resting heart rate is still elevated and as you can see I have not reached pre-COVID training volume yet, but I would say I am recovered. My other states were:
| Pre-COVID | 8 Weeks Post COVID | |
| Total Tonnage Lifted Squat Training % Bench Training % Deadlift Training % | 73,490 lbs 80% 2×2 92.5% 2×2 80% 3×3 | 62,000 lbs 73% 3×6 90% 3×1 83.5% 4×3 |
If my training was not powerlifting specific, I imagine I would still feel somewhat affected based on what I understand about the disease course. I will continue to monitor progress as I make a concerted effort to lower my resting heart rate as a measure of improved cardiovascular health.
But, at this point I feel back to normal.
Note from Mike
I’m really thankful that Alex shared her experienced with us, I think we can all learn from this. As we are quickly learning more about COVID-19, some of what is in this article may not be up to date, please refer to the CDC website for the most recent information. I can’t stress enough that everyone should consult with their physician before starting to exercise after COVID-19. As Alex has learned, COVID impacts the entire body. If you want to reach out to Alex with any questions or if you’re looking for any help, DM her on Instagram.