Today’s guest post is from Ann Wendel on trigger point dry needling and the effect of dry needling for lateral epicondylitis. Dry needling is gaining more popularity and becoming another great option when dealing with trigger points. Ann went through Myopain Seminar’s dry needling certification. I have had the pleasure to get to learn from some of the instructors of the trigger point program, including Katie Adams, and definitely recommend them if this is of interest to you.
Trigger Point Dry Needling
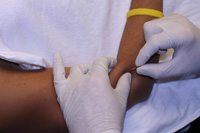
Trigger point dry needling can be used to achieve one of three objectives. First, trigger point dry needling can confirm a clinic diagnosis by relieving the patient’s pain or symptoms of nerve entrapment. Second, inactivation of a MTrP by needling can rapidly eliminate pain in an acute pain condition. Third, inactivation of the MTrP through needling can relax the taut band for hours or days in order to facilitate other therapeutic approaches such as physical therapy and self stretching (Dommerholt and Gerwin, 2006).
Universal precautions are always followed when utilizing dry needling in patient care. During the procedure, a solid filament needle is inserted into the skin and muscle directly at the myofascial trigger point. The trigger point is penetrated with straight in and out motions of the needle. The needle can be drawn back to the level of the skin and redirected to treat other parts of the trigger point not reached in the first pass (Dommerholt and Gerwin, 2006). During this procedure, it is essential to elicit twitch responses in the muscle. The local twitch response (LTR) is an involuntary spinal reflex contraction of muscle fibers within a taut band during needling. Research shows that biochemical changes occur after a LTR, which correlate with a clinically observed decrease in pain and tenderness after MTrP release by dry needling (Shah and Gilliams, 2008).
Trigger Point Dry Needling for Lateral Epicondylitis
Trigger point dry needling is an effective treatment modality for numerous acute and chronic musculoskeletal issues. One condition that responds favorably to dry needling is lateral epicondylitis. Therapists know that this problem has usually become chronic by the time the patient seeks treatment, and progress is usually frustratingly slow for both the patient and the therapist.
When dry needling is incorporated into the treatment plan, results are often seen after 2 or 3 visits. The entire forearm is easily treated with the patient supine on the treatment table, and multiple TrP’s can be treated in a matter of minutes. After a thorough history and physical exam, the therapist assesses the forearm for taut bands and trigger points. Muscles commonly involved in symptoms of lateral epicondylitis include: triceps, brachioradialis, extensor carpi radialis longus (and sometimes brevis), extensor digitorum, anconeus, and supinator. As always, the therapist should screen the neck and shoulder region for MTrP’s. Muscles that may refer pain to the lateral epicondyle include: supraspinatus, infraspinatus, teres major and scalenes.
The needling treatment is completed when all LTR’s are eliminated or the patient requests to stop the treatment. The needle is discarded in a sharps container and hemostasis is applied to the area to decrease bruising. The therapist provides manual therapy with a local stretch to the taut band, myofascial release and therapeutic stretch. The patient is taught a self stretch for home, and the treatment can be concluded with ice or heat to the area. The patient is instructed to stretch the area throughout the day and apply heat/ice as needed. It is not unusual to have some increased soreness at the needling site that may last for up to 48 hours. After 48 hours, most patients report a significant decrease in pain, increase in range of motion and some return of strength.
In conclusion, trigger point dry needling can be used in conjunction with other interventions to treat myofascial pain. At the current time, each state has made its own ruling with regard to the physical therapist’s ability to utilize dry needling. The therapist would be best served by reading the State Practice Act for the state in which they practice to determine their ability to use this modality. I went through 100 hours of classroom and practical training in dry needling and successfully passed both a written and practical exam to become a Certified Myofascial Trigger Point Therapist through Myopain Seminars. I highly recommend this course and I find dry needling to be a very effective part of my practice.
Mike’s Thoughts
Great article Ann, thanks. Dry needling is something I have been exploring and integrating into my practice. I’d love to hear form others about their experiences as well, so please comment below. What works? What technique do you use? What diagnoses respond best?
Here is a video from Youtube for the extensor pollicis brevis. This technique is more aggressive in nature, utilizing and “in and out” pattern of needling rather than just different needles. Different groups teach it differently:
http://www.youtube.com/watch?v=dqu_UGk5ptI

Click the below links for more information:
- Dr. Ma’s Integrated Neuromuscular Trigger Point System
- Dr. Ma’s book Biomedical Acupuncture for Sports and Trauma Rehabilitation: Dry Needling Techniques
- Myopain Seminars’ Dry Needling/Intramuscular Manual Therapy (IMT) Series
References
- Dommerholt, J. and Gerwin, R., Trigger Point Needling Course Manual, The Janet Travell, MD Seminar Series, 2006
- Shah JP, Gilliams EA. Uncovering the biochemical milieu of myofascial trigger points using in vivo microdialysis: an application of muscle pain concepts to myofascial pain syndrome. J Bodyw Mov Ther. Oct 2008;12(4):371-384
- Simons, D.G., Travell, J.G., Simons, L., 1999. Myofascial Pain and Dysfunction: The Trigger Point Manual. Williams & Wilkins, Baltimore.
About the Author
Ann Wendel, PT, ATC, CMTPT holds a B.S. in P.E. Studies with a concentration in Athletic Training from the University of Delaware, and a Masters in Physical Therapy from the University of Maryland, Baltimore. She is a Certified Athletic Trainer (ATC) licensed in Virginia, a Licensed Physical Therapist, and a Certified Myofascial Trigger Point Therapist (CMTPT). Ann received her CMTPT through Myopain Seminars and utilizes Trigger Point Dry Needling as a treatment modality for many pathologies, including lateral epicondylitis.




