
These are not things to be embarrassed about, but rather to grow from. The doctors that used to smoke in the patient rooms 30 years ago, well, that is sort of embarrassing. But who knows, maybe 100 years from now everyone will laugh at us saying, “wow, they used to think the earth was round, they were crazy!!!”
Part of growing is learning and adjusting from past mistakes. The whole “you need to fail before you can learn” concept is true. I hope I can help you cut some corners and you can learn from some of my mistakes!
The 5 most stupid things I didn’t do early in my career
Integrate Soft Tissue Work
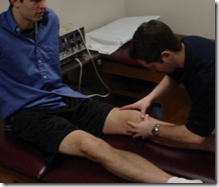
- Soft tissue restrictions can alter the kinematics of the body throughout the kinetic chain.
- Performing soft tissue techniques allows for greater results from other manual techniques you may be performing, such as stretching, joint mobilizations, and even strengthening.
- Hands on time creates a better bond between you and the person you are working with, which in turn leads to better compliance and better outcomes
What do I do now and what can you do to get started? I have personally progressed quite a bit over the last several years. I use a combination of many different techniques including standard deep tissue work, transverse friction, trigger point releases, myofascial release, instrumented-assisted soft tissue, pin and stretch, muscle energy, positional release, etc. They all have a use for different pathologies and all are popular based on my past poll of manual therapy techniques.
I am a believer of an integrated approach. Use as many techniques as you need – try not to have technique tunnel vision!
Understand Movement

Over time I really sought to educate myself in biomechanics, or more specifically for me the understanding of arthrokinematics and joint kinetic forces. You can see this in many of my presentations, writings, and throughout my book The Athlete’s Shoulder. To truly be able to treat a specific joint or injury, you need to understand how the joint(s) should work.
Here is a good example using the shoulder – the person you are assessing has limited elevation with a shoulder “shrug.” Taking the basic understanding I described above, you would likely want to stretch them into elevation, right? Well, yes, and no. You have to understand why the have a shrug, which could be:
- Decreased inferior capsule mobility, causing the humeral head to migrate superiorly away from the area of tightness.
- Insufficient rotator cuff function, losing the dynamic ability of the rotator cuff to central the humeral head during elevation, causing the humeral head to migrate superiorly due to the increased force of the deltoid and the lack of opposing force of the rotator cuff.
As you can see, stretching into elevation would not truly address either of the two proposed mechanisms of the “shrug.” You would need to work on inferior capsular mobility or rotator cuff strength. I spend quite a bit of time discussing some of this as it relates to the shoulder in my online shoulder seminar course.
But this is just a local view of biomechanics, the other view is more global and equally as important, but also keep in mind how other areas in the body impact the joint you are evaluating. Taking this a step further, here are a couple of other reasons why someone may shrug, both further down the kinetic chain:
- Denervation of the long thoracic nerve causing scapular dyskinesis and the loss of the ability to upwardly rotate the scapula, resulting in the humeral head to impingement into the acromion because it can not get out of the way.
- Or maybe a more complicated example – tight hamstrings –> causing a posterior pelvic tilt –> causing a loss of lumbar lordosis –> causing excessive thoracic kyphosis –> causing the common forward head posture with an anterior tilted scapula –> causing a decrease in subacromial space and thus again impingement and shrug because the acromion can’t get out of the way.
As you can see, this global thought process is needed and often overlooked. You may be able to notice the thoracic kyphosis and attempt to treat, that’s great, but keep looking further away to find why the thoracic deviation has occurred. I don’t want to overcomplicate this, but obviously you can see that this approach is pretty neat and exciting when everything starts to click.
I’m not the biggest fan of the thought process that this is the end-all treatment approach, but it is definitely needed. You’ve probably at least heard someone trying to extrapolate the effect of an ingrown toenail on your left foot on right shoulder dysfunction. That may be a bit of a stretch in my mind. Yes, they work together, but don’t overly emphasize.

- The chain reaction is greater the closer to the stone –> the impact of the kinetic chain is greater with the closer joints, or the scapula impacts the shoulder far more than the toe, for example
- The chain reaction is greater when the magnitude of the force is greater (i.e. a bigger rock is thrown) –> An ingrown toenail is going to impact the kinetic chain a lot more than a joint fusion, for example.
As you can see in my photo to the right (that took me like an hour to create, by the way…), A ripple from the hip should have a greater magnitude at the knee and low back than the toe or shoulder. Just my thoughts and experience. I am sure there are always exceptions but this is how I have operated.
This is a huge part of my Champion Performance Specialist program. If we truly want to restore, optimize, and enhance performance, we need to understand how to assess and treat movement dysfunctions.
Understand The Spine
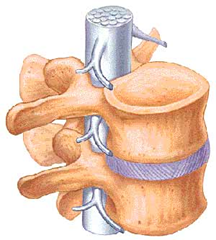
This was really bad for a couple of reasons. One, I missed the larger picture on a few patients. For example, the lateral epicondylitis patient that was actually being referred from the cervical spine. More importantly, it took me a while to truly understand the spine. I had a rudimentary understanding of the spine, but I had no experience.
Luckily, I identified this deficit and addressed it over time. How did I do this? Well, it took some time. I started my quest in understanding the spine by search out books and continuing education courses. I learned a lot, don’t get me wrong, but I continued to lack confidence in my ability to treat the spine. It seemed like everything I was searching for wasn’t there and I would always leave a CEU course or finish a book with the thought, “OK, that’s it…”
It took me some time, but I now realize that you can’t treat the spine like you do the extremities. There isn’t a simple clinical examination process that gives you a fairly definitive diagnosis and subsequent treatment program. The spine is much more gray than black and white. That is why I always felt something was missing after attending a seminar that recommended evaluating a patient, find the patterns of movement that cause symptoms, and then treating accordingly. I would be the person asking, “why?” And I never received a good answer, usually just, “we don’t know why and we don’t care! I just works!” That didn’t sit well with the scientist in me, especially the lack of evidence-based recommendations.

What can you do? Don’t get me wrong, you need to know the foundation behind the spine and classification of dysfunctions etc. You can start with some of the popular groups of thoughts such as Maitland or McKenzie, these are great places to start. But I think you want to quickly advance your understanding of the spine by migrating more towards how the spine works and stabilizes and how to train the spine to work better. I know this is when I made a significant step in the development of my understanding of the spine.
Try these resources below from Stuart McGill and Craig Liebenson, names I am sure you have heard of by now. They do a great job breaking down spine function and treatment based on movement and stability. Once you break free from the thought process of evaluating and treating an injury and focusing more on dysfunctional movement and spine pathology, you’ll see what I mean.
Network Outside My Clique

I spent many years in this position. I learned a lot from my network of like-minded individuals and continue to do so, but those that know me realize that I like to learn from everyone. I attend PT meetings, ATC meetings, CSCS meetings, orthopedic surgeon meetings, everything. I have discussed in the past how much I have learned from collaborating with people from the manual therapy, athletic training, chiropractic, and strength and fitness realms. Understand that everyone has something to offer and learn from everyone. Many people have different perspectives and collaboration is great for you but even better for your patient’s outcomes! It will make you a better clinician in whatever field you choose.
Expand your pool of people to learn from. Try to visit with other people in different disciplines. Read up on some great websites outside of your primary domain, which the strength and fitness groups seem to do so well now. And more importantly, network and collaborate with different groups. You’ll be surprised at how people will challenge some of the basic thoughts that you take for granted.
Share and Learn From My Mistakes
Ah, ego can be a bad thing sometimes, don’t you think? When you are just starting off one of the biggest things you lack (other than experience, of course) is lack of self confidence. I’ve always been a big believer in attitude and the need to always focus on repeating your successes rather than your failures. I recommend reading a good John Maxwell book called The Difference Maker, a book that discusses how your attitude can be your greatest asset. I know, I don’t want to get too much into the “self-help” thing on this website, so take it with a grain of salt if that isn’t your thing.
But reflection is just as important as attitude, as long as you know that you are reflecting to learn from your mistakes rather than dwell on your failure. This is one of the purposes of this series. I am way past the point in my life and career to be embarrassed or too proud to admit mistakes. But this does come back to attitude and self confidence. I know that we all make mistakes and that this is how we learn.
I also think it is important to share my mistakes and recommend you do as well. You will come across many people that may have been through a similar experience and may offer some great advice.
Well, I hope that helped a little. We can all learn from our mistakes, I know I have, and I hope you can learn a little from mine too!




