As our understanding of the mechanics of the shoulder and scapular improve, the reliability and validity of assessing resting scapular position have recently been challenged. Many authors believe that we may be overassessing and assuming dysfunction based on resting scapular position, which would imply that many corrective exercise strategies for the scapula may be either ineffective or inappropriate.
I have really changed how I assess and treat scapular dysfunction over the last decade. My research has led my change in thought process, but other studies have also been reported in the literature.
Does Poor Scapular Position Correlate to Poor Scapular Mobility?
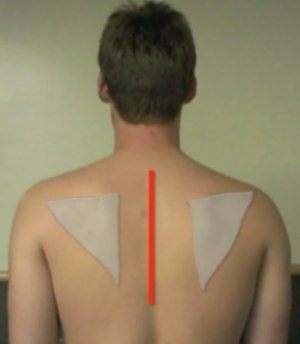
My exploration of scapular asymmetries and dyskinesis led me to first assess scapular position. In baseball players, asymmetries of scapular position are common, and perhaps a normal adaptation.
While these resting static asymmetries were noted, I started to observe that these asymmetries seemed to become much less obvious during active movement. As an example of this, we noted that the resting static position of the scapula on the throwing side was 14mm lower, which was statistically significant. However, when the arms were abducted in the scapular plane to 90 degrees of elevation, the scapula was now symmetrical with the nonthrowing shoulder.
This really made me start thinking about the validity of resting static scapular posture.
To further evaluate this, we then looked at 3D electromagnetic tracking to see if poor static posture correlated to poor scapular mobility, or dyskinesis. We looked at this in a few studies and found that resting static position does not correlate to poor movement patterns.
Several studies have shown that these scapular asymmetries are common in the general population too, so I consider my findings in the overhead athlete relevant to any population. In my experience these same results occur in other populations.
Does Scapular Position Correlate to Injury?
The validity of static resting posture of the scapula has come into recent debate as tests such as the Lateral Scapular Slide Test, described by Kibler, has been shown to find asymmetries in both symptomatic and asymptomatic people. Static postural tests like this have been shown to have both poor reliability and validity, meaning that we are not sure how accurate they are or what these tests actually measure.
Probably more importantly, however, is the finding that static tests have been unable to identify people with and without shoulder injuries, such as in this systematic review from the British Journal of Sports Medicine.
in a 2-year prospective study of over 100 recreational athletes, a recent study in the International Journal of Sports Medicine showed that static resting scapular position did not correlate to the future occurrence of shoulder pain. They did note that the people who developed shoulder pain demonstrated decreased scapular upward rotation at 45 and 90 degrees of elevation, further suggesting that dynamic mobility is more important that static.
These studies are difficult to conduct but it appears that scapular asymmetries are common in the general population and do not correlate to injury. That does not necessarily mean they do not feed into dysfunction, but the correlation may not be as factual as many think.
Recommendations
So what do we know about resting scapular position?
Based on our current understanding of scapular posture, it is hard to place a lot of emphasis on static posture as it does not appear to be reliable, valid, correlate to injury, or correlate to poor movement patterns.
I think one of the worst things you can do is assume dysfunctional movement will occur based on a posture assessment. For example, you would not want to cue excessive scapular movement during arm elevation just because the person is resting in a certain scapular position. You have a very large chance of just further facilitating your compensatory pattern by forcing the motion instead of finding the underlying cause.
People often seem to forget one VERY important fact:
The scapula is part of the scapulothorax joint. The position of the thorax and spine will greatly influence the position of the scapula. [Click to Tweet]
Perhaps an anterior pelvic tilt is causing increased thoracic kyphosis and scapular anterior tilt. Perhaps a forward head posture is causing shortness of the levator scapula and causing downward rotation of the scapula. Cueing movement without addressing the alignment, soft tissue restrictions, and other real issues is going to make this a lot worse.
These are just two examples but hopefully demonstrate the complexity of assessing scapular position and mobility.
To learn more about my approach, I have a recorded webinar for Inner Circle members that reviews how I assess and treat scapular dyskinesis, click here to learn more about my Inner Circle.
Do I still look at posture and scapular position? Sure. I start there, but realize that dynamic movement is likely much more important to assess. I would not recommend that you apply corrective exercises based solely on resting scapular position.