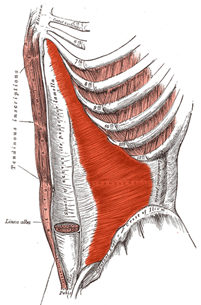
Transversus Abdominis: Are we on the right bandwagon?

What does Transverse Abdominis do?
The function of the TrA is to stabilize the pelvis and low back prior to movement of the body. It acts within a feedforward bilateral muscle activation rationale from spinal perturbations with everyday activities. Rehabilitation is typically aimed at restoring motor control of this key stabilizing muscle. Literature points to effective means of treating low back pain with trunk stabilization and strengthening of deep abdominal musculature to improve motor control1.
Diane Lee gives a great description of how to activate the TrA through abdominal drawing-in maneuver (ADIM)2. However, how long does it take for someone to learn this and do you think they will really do this correctly and efficiently if they are pain? It has been shown that teaching a patient to perform the ADIM maneuver can be time consuming and difficult.3
How effective is activating the Transversus Abdominis?
It has been shown that the TrA is activated after the deltoid (~50ms) with arm movement task studies with LBP patients.4 A recent study showed that during a volitional recruitment task for the TrA , induced pain was shown to attenuate the activity of the TrA.5 It has also been discovered that pain will alter a muscle’s role as an agonist or antagonist to control movement for protection through the pain adaptation model.6 This has also been demonstrated with many prior studies of reduced TrA muscle thickness with chronic LBP. In turn, the delay of TrA timing and optimal muscle activation is altered, potentially making exercises that activate it ineffective when pain is present.
If we abolish the pain, would motor control and activation of TrA resolve itself? There has not been any conclusive data to show that the spine is controlled less when the activation of TrA is changed and altered timing of the TrA leads to poor core stability. The feed-forward activation of TrA can be interpreted differently from a small study that showed 3 of 8 pain-free individuals did not have the feedforward responses in 70% of trials with bilateral arm tasks.7 Even prophylactically, the isolated muscle pattern in pain-free subjects is controversial.8 This goes to show further that low back pain is complex, multimodal and overall challenging to treat.
Is a lack of strength or stability really the reason for the low back pain?
Some thoughts…
As musculoskeletal specialists, we have significant knowledge and a pertinent role in management of low back pain. We need to concentrate on teaching the patients how to control their symptoms independently. To me, this means giving the patient tools to provide self-pain relief through therapeutic means. Activating transverse abdominis stating it will give stability when everyday aches and pains arise just doesn’t seem feasible. The use of foam rolls, towel rolls or any other affordable methods can be very effective in not only giving relief, but obtaining joint motion and allowing an exercise program to be more advantageous. If a treatment doesn’t give someone relief or change, he or she will not be adherent to it, consecutively, returning to health care providers and starting the sequence again.
Since low back pain re-occurs in 70% of cases depending on source, we may not be challenging this problem appropriately. I think having the transversus abdominus as an active component in the treatment is somewhat useful but not conclusive. Pain relieving exercises and education need to be the forefront of each program so muscle activation can be optimal.
What are your opinions? Do you get good results from concentrating on TrA as your main intervention? If so, how effective do you find it and what is your approach? Is there any technique or method that you would recommend others to try?
References
-
- Teyhen DS, Miltenberger CE, Deiters HM, et al.. The use of ultrasound imaging of the abdominal drawing-in maneuver in subjects with low back pain. J Orthop Sports Phys Ther. 2005 Jun;35(6):346-55.
- Accessed 3 March 2009. http://dianelee.ca/services/TRANSVERSUSABDOMINIS.pdf
- O’Sullivan PB, Phyty GD, Twomey LT, Allison GT. Evaluation of specific stabilizing exercise in the treatment of chronic low back pain with radiologic diagnosis of spondylolysis or spondylolisthesis. Spine.1997;22:2959-2967.
- Cresswell AG, Thorstensson A. Changes in intraabdominal pressure, trunk muscle activation and force during isokinetic lifting and lower. Eur J Appl Physio Occup Physiol. 1994; 68: 315-21.
- Kiesel et al. Rehabiliation ultrasound measurement of select muscle activation during induced pain. Manual Therapy. 2008. 13. 132-138
- Lund et al. 1991. The pain adaptation model: a discussion of the relationship between chronic musculoskeletal pain and motor activity. Can J Physiol. Pharmac. 69: 683-694.
- Hodges P, Cresswell A, Thorstennson A. Preparatory trunk motion accompanies rapid upper limb movement. Exp Brain Res 1999;124:69-79.
- Allison GT. The push – throw continuum and core stability – are Physiotherapists teaching the correct motor patterns? in APA National Conference – Sports Physiotherapy Australia. Cairns, Queensland, Australia: 2007.
- Hodges P, Van den Hoorn W, Dawson A, et al. Changes in the mechanical properties of the trunk in low back pain may be associated wtih recurrence. J Biomech. In press.
- Cook C, Hegedus E. Orthopedic Physical Examination Tests: An Evidence-Based Approach. Prentice Hall. 2007.
Flynn, T. (2005). The Use of Ultrasound Imaging of the Abdominal Drawing-in Maneuver in Subjects With Low Back Pain Journal of Orthopaedic and Sports Physical Therapy DOI: 10.2519/jospt.2005.1780
Photos from Wikipedia
Sign up for my FREE newsletter for even more great content!