One of the most important things for any healthcare or fitness professional to understand is that it is our professional duty to our clients to be sure we are staying current and following the evidence as our professions continue to grow. That is what many people believe is evidence-based practice.
I believe this is one of the most important qualities you need to master to truly become an expert in our fields.
We should always be learning and staying on top of the latest research, while keeping an open mind and growth mindset.
Continuing to follow outdated concepts that have been proven to be ineffective or disadvantageous is a disservice to our clients and ultimately our professions.
However, it is very common for students and new graduates to take this concept too far. This is not a criticism, just a statement that without clinical experience it is often difficult to follow evidence based practice as best as possible.
Paralysis by a Lack of Evidence
Here’s one thing that I wish people understood: a lack of evidence does not mean a lack of efficacy.
Research is hard. We’re humans. It’s difficult to have quality randomized control trials with adequate methodology to determine exactly what to do at all times. It’s the expert people that I know that grasp this concept the best.
It’s more common for the inexperienced to have what I call “paralysis by a lack of evidence.” They often state that without clear evidence we should not be performing certain interventions.
This couldn’t be further from the truth in my mind.
What is Evidence Based Practice?
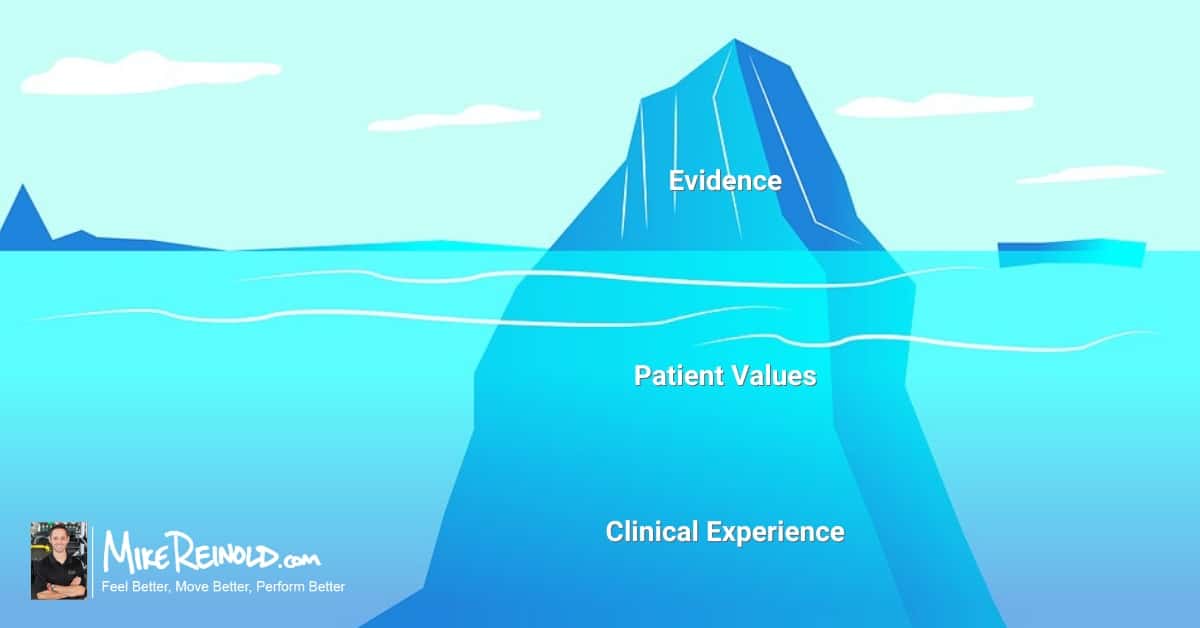
Evidence based practice is defined by Sackett et al as the integration of the current best research evidence with clinical expertise and patient values.
This is super important to grasp. It’s not just the research, it’s also clinical experience and patient values. My friend Phil Page did an excellent job breaking this down in a recent presentation for my Inner Circle Online Mentorship program. Here’s a quick clip from that presentation where Phil defines evidence-based practice, which I thought was brilliant:
I also really liked the iceberg image, representing that EBP isn’t just the best available evidence, but that experience and patient values also lie under the surface.
How to Follow Evidence Based Practice
In order to follow evidence based practice as best as we can, we need to understand that EBP is a combination of these three things. No one piece of this is stronger than another.
When I am trying to determine if an intervention I would like to do is appropriate based on evidence-based practice, I’ll consider what I call the Evidence-Based Practice Light System.
- Red Light = Stop. If there is strong evidence by quality randomized controlled trials suggesting a safety concern or lack of efficacy, then you should find an alternative approach that may be more advantageous.
- Yellow Light = Proceed, but with caution. When there is conflicting information, or there aren’t enough quality studies examining the effect you are assessing, then you must proceed with caution. In this scenario, perhaps there are some low-quality studies (like a case study or publication without strong methodology) that show efficacy, or maybe even some conflicting results in the literature without an overwhelming trend towards efficacy or lack of efficacy.
- Green Light = Go. If there is strong evidence by quality randomized controlled trials suggesting efficacy, then you can comfortably use this approach with evidence-based justification.
We also recently discussed how we do this in a podcast episode on Using Physical Therapy Interventions with No Evidence of Efficacy
If you want to learn more about evidence based practice, you can watch this full presentation and many many more in my Inner Circle Online Mentorship program.