Although the key to successful rehabilitation program for patellofemoral pain requires an accurate differential diagnosis, there are several principles to patellofemoral rehabilitation that should be considered when designing any program. Below are what I would consider the 10 key principles of patellofemoral rehabilitation. They can be used as a backbone to many programs and customized based on the specific diagnosis.
This is part 4 of a series on solving the patellofemoral mystery:
- Part 1: Introduction – Solving the patellofemoral mystery
- Part 2: What causes patellofemoral pain?
- Part 3: Differential diagnosis of patellofemoral pain
- Part 4: Principles of patellofemoral joint rehabilitation
- Part 5: Specific treatment guidelines for patellofemoral pain
- Part 6: Biomechanics of the patellofemoral joint – clinical implications
- Part 7: Understanding the clinical implications of the kinetic chain: The influence of the hip and foot on the patellofemoral joint
1. Reduce Swelling
The first principle of patellofemoral rehabilitation is the reduction of swelling. Patellofemoral patients often present with joint effusion following injury and postoperatively. Chronic edema may also exist due to repetitive microtrauma of the soft tissues surrounding the patellofemoral joint.
Numerous authors have studied the effect of joint effusion on muscle inhibition. DeAndrade et al (JBJS 1965) were the first to report in the literature that joint distention resulted in quadriceps muscle inhibition. A progressive decrease in quadriceps activity was noted as the knee exhibited increased distention. Spencer et al (Archive Phys Med Rehab 1984) found a similar decrease in quadriceps activation with joint effusion. The authors reported the threshold for inhibition of the vastus medialis to be approximately 20-30ml of joint effusion and 50-60ml for the rectus femoris and vastus lateralis. This is really not a lot of fluid, so any amount of effusion is significant. An unpublished study by Bob Mangine in the 1990’s showed that just a 30-40ml increase in fluid to the knee resulted in almost a 50% drop in quadriceps peak torque.

2. Reduce Pain
The second principle of patellofemoral rehabilitation is the reduction of pain. Pain may also play a role in the inhibition of muscle activity observed with joint effusion. Young et al (MSSE 1983) examined the electromyographic activity of the quadriceps in the acutely swollen and painful knee. An afferent block by local anesthesia was produced intraoperatively during medial meniscectomy. Patients in the control group reported significant pain postoperatively and pronounced inhibition of the quadriceps (30-76%). In contrast, patients with local anesthesia reported minimal pain and only mild quadriceps inhibition (5-31%).
Pain can be reduced passively through the use of cryotherapy and analgesic medication. Immediately following injury or surgery, the use of a commercial cold wrap, such as a DonJoy Iceman, can be extremely beneficial. Passive range of motion may also provide neuromodulation of pain during acute or exacerbated conditions. Various other therapeutic modalities such as ultrasound and electrical stimulation may also be used to control pain via the gate control theory if that is your belief.
3. Restore Volitional Muscle Control

Snyder-Mackler et al (JBJS 1991) examined the effect of electrical stimulation on the quadriceps and musculature during 4 weeks of rehabilitation following ACL reconstruction. The authors noted that the addition of neuromuscular electrical stimulation to postoperative exercises resulted in stronger quadriceps and more normal gait patterns than patients exercising without electrical stimulation. Delitto et al (PT 1988) and Snyder-Mackler et al (JBJS 1995) reported similar results of both the quadriceps and hamstrings using electrical stimulation for a 3-week and 4-week, respectively, training period following ACL reconstruction.
The use of electrical stimulation and biofeedback on the quadriceps musculature appears to facilitate the return of muscle activation and may be valuable additions to therapeutic exercises. Clinically, I use electrical stimulation immediately following injury or surgery while performing isometric and isotonic exercises such as quadriceps sets, straight leg raises, hip adduction and abduction, and knee extensions. I also use this as a maintenance program with many of my athletes with chronic knee issues.
4. Emphasize the Quadriceps
The next principle of patellofemoral rehabilitation is to strengthen the knee extensor musculature. Some authors have recommended emphasis on enhancing the activation of the VMO in patellofemoral patients based on reports of isolated VMO insufficiency and asynchronous neuromuscular timing between the VMO and VL.

Several interventions and exercise modifications have been advocated to effectively increase the VMO:VL ratio, based mostly on anecdotal observations. These include hip adduction, internal tibial rotation, and patellar taping and bracing. Powers(JOSPT 1998) reports that isolation of VMO activation may not be possible during exercise, stating that several studies have shown that selective VMO function was not found during quadriceps strengthening exercises, exercises incorporating hip adduction, or exercises incorporating internal tibial rotation. Powers also states that although the literature offers varying support for VMO strengthening, successful clinical results have been found while utilizing this treatment approach.
My belief is that quadriceps strengthening exercises should be incorporated into patellofemoral rehabilitation programs. Strength deficits of the quadriceps may lead to altered biomechanical properties of the patellofemoral and tibiofemoral joints. Any change in quadriceps force on the patella may modify the resultant force vector produced by the synergistic pull of the quadriceps and patellar tendons, thus altering contact location and pressure distribution of joint forces. Furthermore, the quadriceps musculature serves as a shock absorber during weightbearing and joint compression, any abnormal deviations in quadriceps strength may result in further strain on the patellofemoral and/or tibiofemoral joint.
In reality, I believe that quadriceps strengthening is very important for patellofemoral rehabilitation, but many exercises designed to “enhance VMO” strength or activation may actually be disadvantageous to the joint. Take for example the classic squeezing of the ball during closed kinetic chain exercises such as squatting and leg press. This creates an IR and adduction moment at the hip that is now known to be detrimental to patellofemoral patients. I would actually propose that we work on quadriceps strengthening without an adduction component and rather emphasize hip adbuction and external rotation. This can be performed with the use of a piece of exercise band around the patient’s knees during these exercises. We will get into this in more detail in an upcoming post in this series.
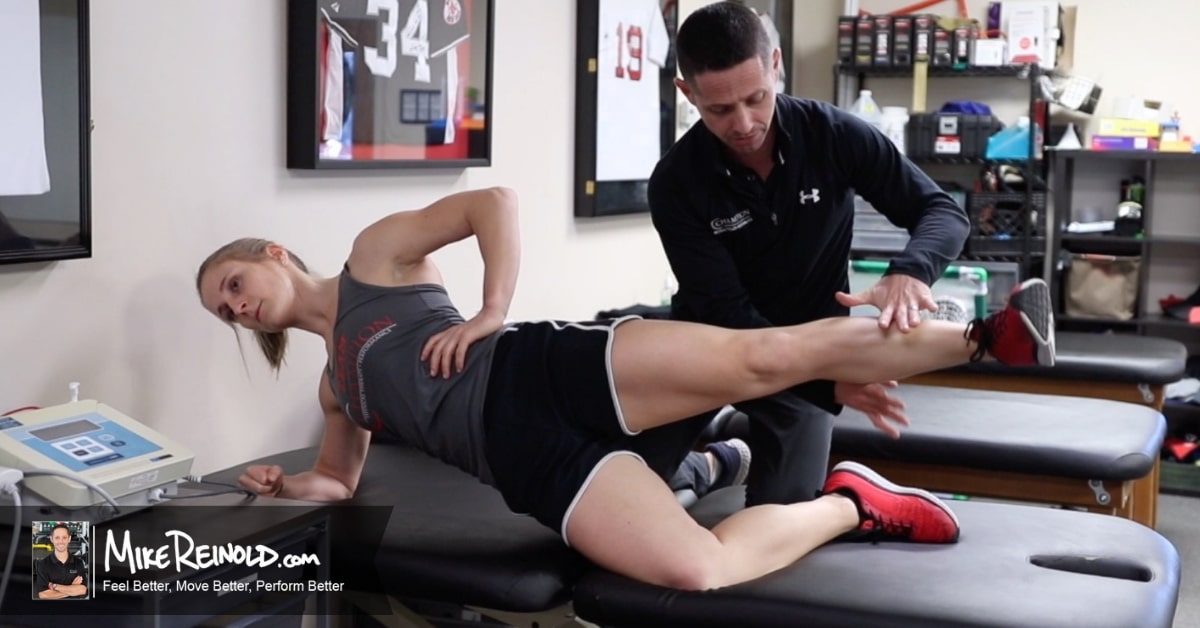
5. Control the Knee Through the Hip

Emphasize the hip’s ability to eccentrically control the valgus moment at the knee produced by hip IR and adduction. I can’t say it enough, work on hip abduction and ER. This tip alone will greatly enhance your patellofemoral outcomes. More on this in a future post.
6. Enhance Soft Tissue Flexibility
Another principle of patellofemoral rehabilitation is the enhancement of joint flexibility with emphasis on quadriceps, hamstrings, hip adductors, gastrocnemius, and iliotibial band stretching. Any deficit in flexibility of these areas will cause significant biomechanical faults throughout the kinetic chain.
Rehabilitation should focus on restoring full passive knee extension initially to minimize the development of a flexed knee posture exhibited by some patients with patellofemoral disorders. Ambulating and performing daily activities with a knee flexion contracture may result in increased patellofemoral joint reaction forces and requires a great deal of motor control to stabilize the knee joint. Full passive knee extension is important for improved quadriceps activity and also allows the knee to lock out while standing, thus allowing relaxation of the surrounding musculature.
Restoring full knee flexion is also a significant priority. In postoperative patients, knee flexion is gradually restored especially in the presence of an effusion. In non-operative patients, knee flexion is gradually restored through controlled stretching exercises. The goal of restoring full knee flexion is not merely reestablishing quadriceps flexibility but improving soft tissue flexibility of the retinacular tissues as well.
Witvrouw et al (AJSM 2000) prospectively studied the risk factors for the development of anterior knee pain in the athletic population over a 2-year period. A significant difference was noted in the flexibility of the quadriceps and gastrocnemius muscles between the group of subjects that developed patellofemoral pain and the control group, suggesting that athletes exhibiting tight musculature may be at risk for the development of patellofemoral disorders.
7. Improve Soft Tissue Mobility

While taping of the patella has received conflicting reports in the literature regarding its efficacy for correcting biomechanical deficits of the patella, taping may assist in restoring soft tissue flexibility by providing a low-load prolonged stretch of the retinacular tissues. Study after study shows that tape does not impact patella position or tracking (don’t get me wrong there are some that show that it does, but there are more that says tape does not). My personal belief is that this is the reason for a reduction in symptoms with the application of tape. Remember that the source of patellofemoral pain may not be from the articular cartilage but rather from the retinacular tissue.
The utilization of a brace which imparts a medial glide or force to the patella may also be beneficial. There are many on the market and I truly have no preference at this time. It seems like a new and improved brace comes out every 6 months. Preliminary MRI studies have documented the effectiveness of bracing.
8. Enhance Proprioception and Neuromuscular Control
Rehabilitation programs must also include drills designed to restore proprioceptive and neuromuscular control skills in patellofemoral patients. Proprioception and postural balance training begins immediately postinjury or postoperatively. Specific drills initially include weight shifting side-to-side, weight shifting diagonally, mini-squats, and mini-squats on an unstable surface such as a tilt board. As the patient advances, tilt board squats can be progressed from double leg to single leg.
Perturbations can further be added to challenge the neuromuscular system. Initially, the clinician can apply manual perturbations. As the patient sustains a vertical squat on a tilt board at 30 degrees of knee flexion, the clinician adds perturbations by tapping the board with his or her foot.
Ball tosses can be incorporated with manual perturbations to provide additional challenge. The patient progresses to perform a vertical squat to 30 degrees of knee flexion while performing a chest-pass with a 3-5 pound weighted ball. The rehabilitation specialist continues to add manual perturbations by tapping the board. Ball throws are progressed from chest-passes to side-to-side throws, and then overhead soccer throws. Again, these exercises can be progressed from double-leg to single-leg stance to further challenge the patients neuromuscular control.
Depending on their sport participation, jump and landing training may also be necessary to teach the athlete how to avoid detrimental positions.
9. Normalize Gait
Gait training is also a critical component to patellofemoral rehabilitation. A variety of factors contribute to antalgic and inefficient gait patterns including joint effusion, pain, soft tissue tightness, and scar tissue formation.
Strategies used to minimize the flexed knee gait pattern that is commonly exhibited by patellofemoral patients include minimizing joint effusion and enhancing sift tissue flexibility, particularly the hamstring and gastrocnemius musculature. Specific techniques include retrograde walking over cones. This particular exercise requires adequate quadriceps control and involves the patient ambulating while high stepping over successive cones. As the patient moves backward, the foot strikes the ground in a toe to heel pattern to produce an extension moment at the knee.
10. Gradually Progress Back to Activities
Lastly, as the patellofemoral patient progresses through the rehabilitation program, emphasis should shift towards functional activities that replicate activities specific to each patient. The rate of progression with functional activities is dictated by the patient’s unique tolerance to the activities. Exercise must be performed at a tolerable level without overstressing the healing tissues. Pathological loading that produces detrimental stress on the patellofemoral joint should be avoided to prevent exacerbations of symptoms. Functional stresses are gradually increased leading to a steady return to function. The functional progression of activities should follow a progressive and sequential order to ensure proper amounts of stress are applied to facilitate healing without producing disadvantageous forces.
I hope that these principles are helpful in establishing a proper and comprehensive treatment program. Next post will focus on specific treatments for each diagnosis previously discussed based on the classification of patellofemoral pain. As always, I would love to hear your thoughts on what other principles you feel are important. I am sure there are some thoughts on bracing and taping. In my experience, the benefits have been limited but I am eager to hear your thoughts as I am sure there are many of you with far more experience with these techniques than myself.
Continue reading to Part 5: Specific Treatment Guidelines for Patellofemoral Pain
WANT TO LEARN MORE FROM ME?
Subscribe to my newsletter to get my best articles, plus you'll also get FREE access to my new Introduction to Performance Therapy & Training online course

We take our privacy seriously and will never share your information.